
Bone tuberculosis is a serious form of extrapulmonary tuberculosis that affects the bones and joints rather than the lungs. Although tuberculosis is commonly associated with pulmonary infection, skeletal involvement can lead to long-term complications if not diagnosed and treated early. In India and other developing countries, the burden of bone tuberculosis remains clinically significant, particularly in individuals with weakened immunity.
This comprehensive guide explains the causes, risk factors, clinical presentation, diagnostic pathway, and modern bone tuberculosis treatment options in a structured, evidence-based manner.
Bone tuberculosis is a chronic bacterial infection caused by Mycobacterium tuberculosis that spreads from the lungs or other primary sites to the skeletal system through the bloodstream. It most commonly affects the spine, hips, knees, and long bones.
The condition is also known as:
When the spine is involved, it is referred to as Spinal tuberculosis, historically called Pott’s disease. When joints are affected, it is termed Joint tuberculosis.
Bone tuberculosis occurs when tuberculosis bacteria disseminate hematogenously from a primary focus, usually pulmonary TB. In some cases, the primary infection may be latent or asymptomatic.
Individuals living in TB-endemic regions are at higher risk.
Spinal tuberculosis accounts for nearly 50% of skeletal TB cases. It commonly affects the thoracic and lumbar vertebrae.
Clinical features include:
If untreated, spinal tuberculosis may cause spinal cord compression.
Joint tuberculosis typically affects weight-bearing joints such as:
This form presents as chronic monoarthritis with gradual joint destruction.
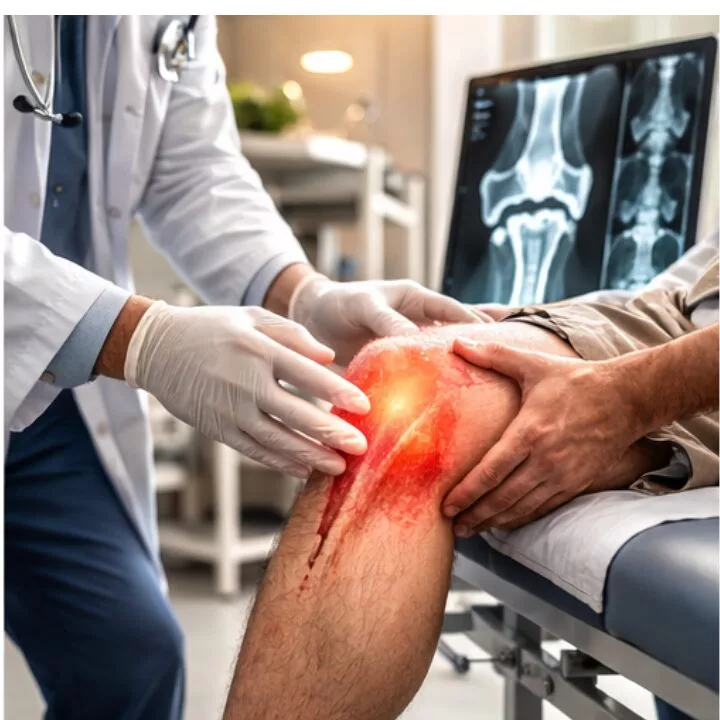
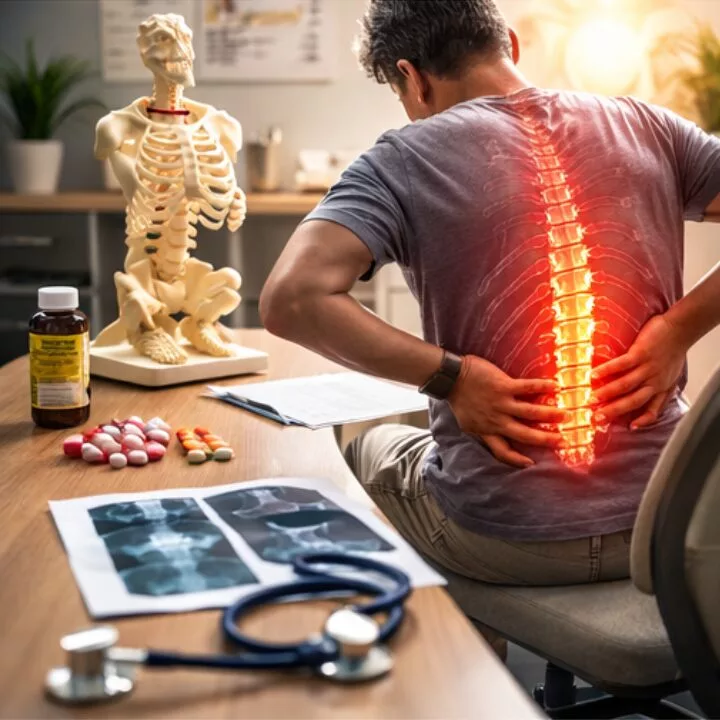
Understanding bone tuberculosis symptoms and treatment options early can significantly improve prognosis.
Bone tuberculosis symptoms develop gradually and may include:
In spinal tuberculosis:
Because symptoms are slow and nonspecific, diagnosis is often delayed.
Avoid activities that worsen the stiffness. Giving your muscles time to recover is essential.
A common concern among patients is: is bone tuberculosis communicable?
Bone tuberculosis itself is not directly contagious through casual contact. However, if the individual also has active pulmonary TB, the lung infection can be transmissible via respiratory droplets.
Therefore:
Early diagnosis and complete treatment significantly reduce infectivity.
Timely diagnosis is critical to prevent irreversible bone damage.
Orthopedic evaluation focuses on:
Neurological assessment in spinal cases
Timely diagnosis is critical to prevent irreversible bone damage.
Biopsy remains the confirmatory test for bone tuberculosis.
Bone tuberculosis treatment primarily involves long-term anti-tubercular therapy (ATT). Early initiation improves outcomes and reduces complications.
Standard bone tuberculosis treatment includes:
Treatment duration:
Compliance is essential to prevent drug resistance.
Surgery is indicated when:
Procedures may include:
Not all cases require surgery; most respond to medical therapy alone.
Recovery from bone tuberculosis depends on:
Patient immunity
Physiotherapy plays a vital role in restoring joint mobility.
Delayed or inadequate treatment may result in:
Early bone tuberculosis treatment prevents these outcomes.
Preventive strategies include:
Feature | Bone Tuberculosis | Arthritis |
Cause | Bacterial infection | Autoimmune or degenerative |
Fever | Common | Rare |
Weight loss | Present | Absent |
Duration | Gradual | Variable |
Treatment | Anti-TB drugs | Anti-inflammatory drugs |
Proper diagnosis prevents mismanagement.
Preventive strategies include:
Bone tuberculosis is a chronic but treatable infectious condition affecting the skeletal system. Early recognition of bone tuberculosis symptoms and treatment initiation are crucial to prevent long-term disability. With modern diagnostic tools and prolonged anti-tubercular therapy, outcomes are significantly improved. Awareness, timely intervention, and adherence to treatment protocols remain the cornerstone of effective bone tuberculosis management.