Knock Knees Treatment in Adults & Children: Complete Care and Solutions

Knock Knees Treatment in Adults & Children: Complete Care and Solutions Home / Knock knees, medically known as Genu Valgum, is a common knee alignment condition where the knees touch each other while the ankles remain apart. This condition can affect both children and adults, leading to discomfort, walking issues, and long-term joint complications if not treated properly. In this comprehensive guide, we will explain everything about knock knees treatment, including causes, symptoms, diagnosis, and the best care options available today. What is Knock Knees Treatment? Knock knees treatment refers to a range of medical and non-medical approaches used to correct abnormal knee alignment. The goal is to: Improve leg alignment Reduce pain and discomfort Prevent joint damage Restore normal walking patterns Knock knees treatment depends on age, severity, and underlying causes. Children often improve naturally with growth, while adults may need structured physiotherapy, lifestyle changes, or surgical correction for proper alignment. Causes of Knock Knees Understanding the cause is essential for selecting the right knee treatment approach. Common Causes in Children Natural growth variations (physiological genu valgum) Nutritional deficiencies like Rickets Genetic conditions Bone development disorders Causes in Adults Previous injuries (Knee Injury) Arthritis such as Osteoarthritis Obesity causing excess pressure on joints Improper healing of fractures Other Contributing Factors Weak muscles around the knee Poor posture Lack of physical activity Symptoms of Knock Knees Symptoms of knock knees vary by severity and age, including knees touching while standing, gap between ankles, walking difficulty, knee pain, joint stiffness, and in severe cases, imbalance and posture issues.. Common Signs Knees touching while standing straight Gap between ankles Difficulty walking or running Frequent tripping in children Pain-Related Symptoms Persistent knee pain treatment needs Joint stiffness Swelling around knees Discomfort after long standing Advanced Symptoms Uneven walking pattern Hip or ankle pain Increased risk of joint degeneration Risk Factors Certain individuals are more prone to developing knock knees: Obesity or excess body weight Family history of bone deformities or certain orthopedic disability conditions Poor nutrition (low calcium & vitamin D) Previous knee injury treatment history Sedentary lifestyle Weak thigh and hip muscles Children who start walking too early or have poor posture may develop knock knees, as their bones and joints are still growing and more prone to alignment issues during early developmental stages. Diagnosis and Medical Tests Accurate diagnosis is crucial for effective knock knees treatment adults and children. Physical Examination Doctors check: Knee alignment Walking pattern (gait analysis) Distance between ankles Imaging Tests X-rays: To evaluate bone structure MRI scans: For soft tissue damage CT scans: In complex cases Advanced Assessment Joint function tests Muscle strength evaluation Alignment measurements Diagnosis and tests help doctors decide the right treatment approach, whether non-surgical methods like physiotherapy and exercises or surgical correction, ensuring effective knee joint pain treatment and proper alignment.. Treatment Options Treatment depends on age, severity, and underlying cause. 1. Non-Surgical Treatment (First Line Approach) a) Knock Knees Treatment Exercise Exercise plays a key role in correcting alignment. Recommended exercises: Squats (improve thigh strength) Leg raises Clamshell exercise Resistance band walking Yoga for posture correction These knock knees treatment exercise methods strengthen muscles around the knee and improve alignment gradually. b) Physiotherapy Improves mobility and flexibility Strengthens quadriceps and hamstrings Corrects walking posture Physiotherapy is one of the best treatment for knee pain and alignment issues. c) Weight Management Reduces stress on knees Improves recovery Prevents worsening of deformity d) Orthotics and Braces Knee braces help maintain alignment Shoe inserts improve walking balance 2. Medical Treatment Doctors may recommend: Pain relief medications Anti-inflammatory drugs Supplements (calcium, vitamin D) These support knee treatment but do not correct alignment alone. 3. Surgical Treatment For severe cases, surgery may be required. Types of Surgery Guided growth surgery (for children) Osteotomy (bone realignment) Knee replacement (in advanced adults with arthritis) Surgery is usually recommended when: Pain is severe Mobility is restricted Non-surgical methods fail Knock Knee Treatment for Child Children often improve naturally as they grow. However, treatment may include: Observation and regular monitoring Physical therapy Nutritional support Bracing in some cases Early diagnosis ensures better outcomes. Knock Knees Treatment Adults In adults, correction is more complex and may include: Structured physiotherapy Lifestyle modifications Advanced surgical options Timely intervention prevents complications like joint damage. Recovery and Rehabilitation Recovery depends on the type of treatment. After Non-Surgical Treatment Regular exercise routine Gradual improvement in alignment Pain reduction within weeks After Surgery Rehabilitation program for 6–12 weeks Physiotherapy for strength recovery Limited movement initially Full recovery may take 3–6 months Consistency is key for successful recovery. Prevention Tips Preventing knock knees is possible with simple lifestyle changes: Maintain a healthy weight Eat calcium and vitamin D-rich foods Stay physically active Practice good posture Strengthen leg muscles regularly Early intervention is the best prevention strategy. When to See a Doctor Consult a specialist if: Knee pain persists for weeks Walking becomes difficult Knees worsen over time Child’s condition does not improve after age 7 Visible deformity increases Timely medical care helps ensure effective knee joint pain treatment, improves mobility, reduces discomfort, and prevents long-term complications like joint damage, deformity progression, and difficulty in daily activities. Frequently Asked Questions (FAQs) Can knock knees be corrected without surgery? Yes, mild to moderate cases can be corrected with exercises, physiotherapy, and lifestyle changes. What is the best exercise for knock knees? Squats, leg raises, and resistance band exercises are highly effective for improving alignment. Is knock knees normal in children? Yes, it is common in young children and often corrects naturally by age 7. When is surgery needed for knock knees? Surgery is required in severe cases where pain, deformity, or mobility issues persist. Can knock knees cause long-term problems? Yes, untreated cases can lead to joint pain, arthritis, and walking difficulties. Conclusion Knock knees is a manageable condition when diagnosed early and treated correctly. Whether it’s a child or an adult, proper care, exercises, and medical guidance can significantly improve alignment and quality of life. From knock knees treatment
L5-S1 Disc Bulge: Causes, Symptoms, and Effective Treatment Options
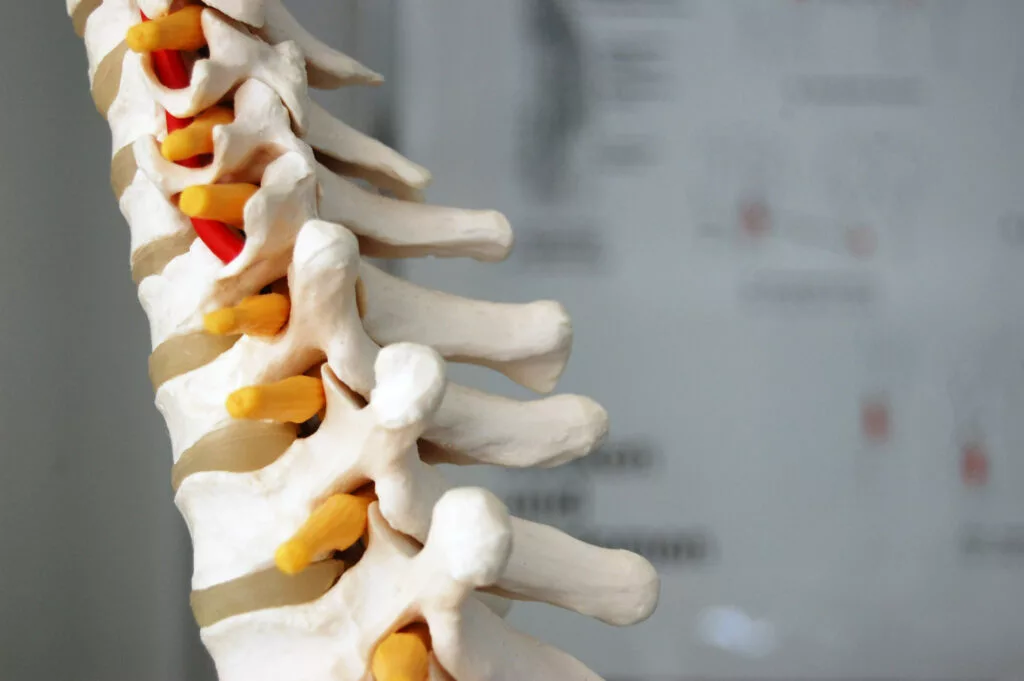
L5-S1 Disc Bulge: Causes, Symptoms, and Effective Treatment Options Home / Lower back pain has become increasingly common due to modern lifestyles, especially among people with desk jobs and limited physical activity. One of the most frequent causes of chronic lower back pain is an L5-S1 disc bulge. This condition can lead to discomfort, restricted movement, and even nerve-related symptoms if not treated on time. Understanding its causes, symptoms, and treatment options can help you take the right steps toward recovery. What is an L5-S1 Disc Bulge? The L5-S1 segment is located at the lowest part of the spine, where the lumbar spine (L5 vertebra) meets the sacrum (S1). It is one of the most stressed areas of the spine, as it bears a significant amount of body weight. A disc bulge occurs when the intervertebral disc extends beyond its normal boundary. This can put pressure on nearby nerves, leading to pain and other symptoms. Causes of L5-S1 Disc Bulge Several factors can contribute to the development of an L5-S1 disc bulge: Age-related degeneration of spinal discs Prolonged sitting and sedentary lifestyle Poor posture, especially during work or screen time Heavy lifting or sudden strain Injury or trauma Obesity, which increases pressure on the spine With increasing screen time and reduced physical activity, this condition is becoming more common among young adults as well. Common Symptoms The symptoms of an L5-S1 disc bulge can vary depending on the severity: Persistent lower back pain Pain radiating to the hips, buttocks, or legs (commonly known as sciatica) Tingling or numbness in the legs or feet Muscle weakness Difficulty in sitting, bending, or standing for long periods In severe cases, it may interfere with walking or daily activities. Diagnosis Accurate diagnosis is essential for effective treatment. Doctors may recommend: Physical examination to assess movement and pain levels MRI scan, which is the most reliable method to detect disc bulges X-rays to evaluate bone structure Early diagnosis significantly improves treatment outcomes. Effective Treatment Options 1. Non-Surgical Treatment (First-Line Approach) In most cases, L5-S1 disc bulge can be treated without surgery: Pain-relief medications Physiotherapy and guided exercises Posture correction techniques Lifestyle and activity modifications Nearly 70–80% of patients recover with conservative treatment. 2. Advanced Non-Surgical Treatments If symptoms persist, advanced treatments may be recommended: Epidural steroid injections to reduce inflammation Specialized spine rehabilitation programs 3. Surgical Treatment (For Severe Cases) Surgery is considered only when non-surgical methods fail or nerve compression becomes severe: Microdiscectomy Minimally invasive or endoscopic spine surgery These procedures are designed to relieve nerve pressure and restore function. Prevention Tips Preventing an L5-S1 disc bulge is possible with simple lifestyle changes: Maintain proper posture while sitting and standing Engage in regular exercise and core strengthening Avoid prolonged sitting; take frequent breaks Maintain a healthy body weight Use proper techniques while lifting heavy objects When to See a Doctor Consult a spine specialist if you experience: Back pain lasting more than 1–2 weeks Pain radiating down the leg Increasing numbness or weakness Difficulty performing daily activities Early medical intervention can prevent complications. Frequently Asked Questions (FAQs) What is an L5-S1 disc bulge? An L5-S1 disc bulge is a condition where the spinal disc between the L5 and S1 vertebrae extends beyond its normal position, potentially pressing on nearby nerves and causing pain or discomfort. Is an L5-S1 disc bulge serious? In most cases, it is not serious and can be treated with non-surgical methods. However, if left untreated, it may lead to nerve compression and worsening symptoms. What are the main symptoms of an L5-S1 disc bulge? Common symptoms include lower back pain, leg pain (sciatica), numbness, tingling, and muscle weakness. The severity depends on nerve involvement. Can an L5-S1 disc bulge heal on its own? Yes, many cases improve with rest, physiotherapy, and lifestyle changes. The body can naturally reduce inflammation over time. How long does it take to recover from an L5-S1 disc bulge? Recovery time varies but usually takes 4 to 8 weeks with proper treatment. Severe cases may take longer. Conclusion An L5-S1 disc bulge is a common yet manageable condition. With timely diagnosis and the right treatment approach, most patients can return to a pain-free and active life. If you are experiencing persistent lower back pain or sciatica symptoms, do not ignore them. Seek expert care and start your recovery journey today.
Which Size of Gallbladder Stone is Dangerous? Warning Signs You Should Not Ignore
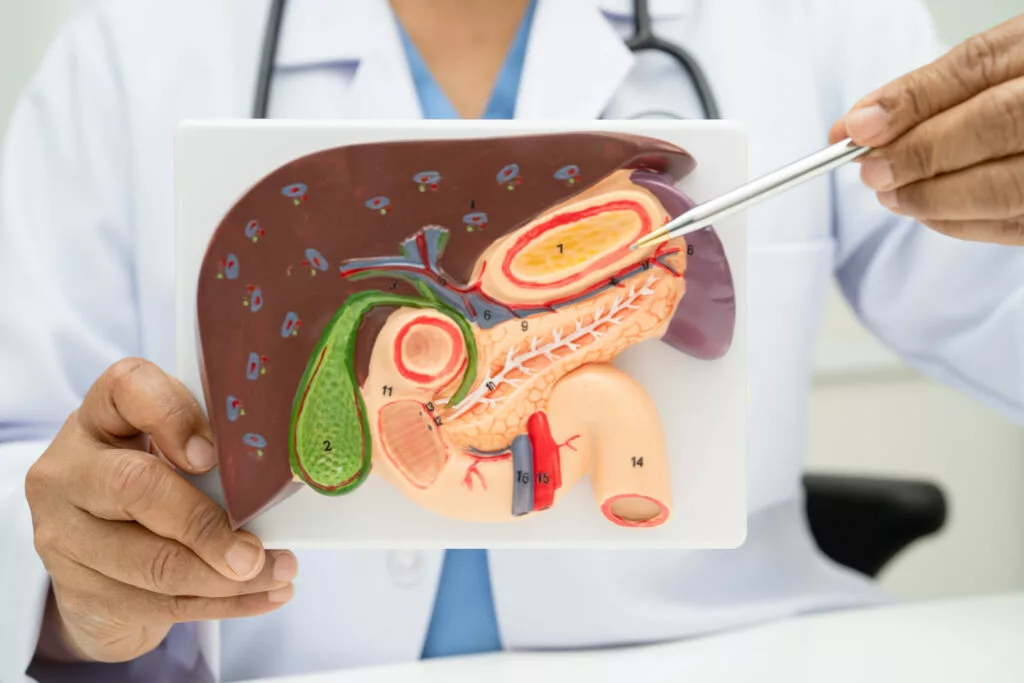
Which Size of Gallbladder Stone is Dangerous? Warning Signs You Should Not Ignore Home / Gallbladder stones are a common health problem that affects many people, especially adults. But one question that often worries patients is: which size of gallbladder stone is dangerous? The answer is not always simple, because both small and large stones can create serious health issues depending on their location and symptoms. In this detailed guide, we will explain everything you need to know about which size of gallbladder stone is dangerous, along with causes, symptoms, risks, and treatment options in simple and easy language. Which Size of Gallbladder Stone is Dangerous? When discussing which size of gallbladder stone is dangerous, it is important to understand that danger is not only based on size but also on movement and blockage. Small Stones (Less than 5 mm) Small stones may seem harmless However, they can easily move into bile ducts This can cause blockage and severe complications Small gallbladder stones are often more dangerous because they can easily move into the bile ducts and cause blockage. This can lead to severe pain, infection, jaundice, or even pancreatitis, making timely diagnosis and treatment very important. Medium Stones (5 mm – 10 mm) These stones may cause pain and discomfort They may or may not move Risk depends on symptoms and position Large Stones (More than 10 mm) Large stones usually stay in the gallbladder They may cause inflammation or infection Less likely to block ducts but still risky Gallbladder Stone Reason (Causes) Gallbladder stones form due to excess cholesterol, bile imbalance, or poor gallbladder emptying. Common causes include obesity, unhealthy diet, rapid weight loss, diabetes, and hormonal changes. These factors increase the risk of developing gallbladder stones over time. Excess cholesterol in bile Obesity or sudden weight loss Poor diet (high fat, low fiber) Diabetes Hormonal changes (especially in women) Family history These factors increase the chances of developing gallbladder stones over time by affecting bile composition and flow. When cholesterol or waste substances build up, they can form solid particles inside the gallbladder, leading to stone formation and possible digestive complications later. Gallbladder Stone Symptoms You Should Not Ignore Recognizing gallbladder stone symptoms early can prevent serious complications. Common Symptoms: Severe pain in the upper right abdomen Pain after eating fatty food Nausea and vomiting Bloating and gas Fever (in case of infection) Serious Warning Signs: Yellowing of skin (jaundice) Persistent vomiting High fever with chills Sudden intense pain lasting for hours These warning signs indicate that you should seek medical help immediately. Why Size Matters in Gallbladder Stones The question which size of gallbladder stone is dangerous is important because: Small stones can block bile ducts Large stones can cause chronic irritation Multiple stones increase overall risk Doctors usually evaluate: Size Number of stones Symptoms Patient’s overall health Complications of Gallbladder Stones If left untreated, gallbladder stones can lead to serious problems: 1. Gallbladder Inflammation (Cholecystitis) Severe pain and swelling Requires immediate treatment 2. Bile Duct Blockage Causes jaundice Can lead to liver problems 3. Pancreatitis Inflammation of pancreas Life-threatening condition Gallbladder Stones Treatment Options There are different types of gallbladder stones treatment depending on severity. 1. Medication Used for small stones Helps dissolve stones slowly Not always effective 2. Lifestyle Changes Low-fat diet Weight management Regular exercise 3. Gallbladder Stone Operation When symptoms are severe, doctors recommend a gallbladder stone operation. Types of Surgery: Laparoscopic surgery (minimally invasive) Open surgery (in complicated cases) Gallbladder Stone Surgery Gallbladder stone surgery is the most effective treatment when: Stones are causing pain There are complications Stones are large or multiple During surgery, the gallbladder is removed, which is safe and does not affect digestion significantly. Gallbladder Stone Surgery Cost The gallbladder stone surgery cost can vary depending on: Hospital type City Surgeon’s experience Type of surgery In India, the cost usually ranges between ₹40,000 to ₹1,20,000 (approx). Real Gallbladder Stone vs Symptoms Sometimes people confuse gas or acidity with stones. A real gallbladder stone problem usually includes: Repeated pain episodes Pain after meals Confirmed diagnosis through ultrasound When Should You See a Doctor? You should consult a doctor if: Pain occurs frequently Symptoms worsen over time There is fever or jaundice Pain does not go away Early diagnosis helps avoid serious complications. How to Prevent Gallbladder Stones Prevention is always better than treatment. Follow these tips: Maintain a healthy weight Avoid oily and junk food Eat fiber-rich foods Stay hydrated Exercise regularly Which Size of Gallbladder Stone is Dangerous – Final Understanding To summarize: Small stones → more dangerous due to movement Large stones → risky due to inflammation Medium stones → moderate risk So, the real answer to which size of gallbladder stone is dangerous depends on symptoms and complications, not just size. Frequently Asked Questions (FAQs) Which size of gallbladder stone is dangerous? Small stones are often more dangerous because they can block bile ducts, while large stones can cause long-term inflammation. Can small gallbladder stones be serious? Yes, small stones can move into bile ducts and cause severe complications like blockage and pancreatitis. What are the main gallbladder stone symptoms? Common symptoms include abdominal pain, nausea, vomiting, and pain after eating fatty food. Is surgery necessary for gallbladder stones? Surgery is recommended if stones cause pain, infection, or complications. When is dialysis required for kidney disease? Most patients recover within 1–2 weeks after laparoscopic surgery. Conclusion Understanding which size of gallbladder stone is dangerous is essential for timely treatment and prevention of complications. Both small and large stones have risks, and ignoring symptoms can lead to serious health problems. If you experience any warning signs, do not delay medical consultation. Early diagnosis and proper treatment can help you stay healthy and avoid complications.
Can Kidney Disease Be Cured? Understanding the Truth About Kidney Health
Can Kidney Disease Be Cured? Understanding the Truth About Kidney Health Home / Kidneys play a vital role in keeping our body healthy and functioning properly. These two bean-shaped organs are responsible for filtering waste products, removing excess fluids, balancing minerals, and maintaining overall body health. However, when the kidneys are damaged or stop functioning effectively, it can lead to kidney disease. One of the most common questions patients ask is: Can kidney disease be cured? The answer depends on the type, stage, and cause of the disease. While some kidney conditions can be treated and reversed in the early stages, others may require long-term management rather than a complete cure. Understanding kidney disease and taking timely action can help prevent serious complications. Understanding Kidney Disease Kidney disease occurs when the kidneys lose their ability to filter blood properly. This results in the buildup of waste, toxins, and excess fluids in the body. Kidney disease can develop slowly over time or occur suddenly depending on the underlying cause. There are two main types of kidney disease: 1. Acute Kidney Injury (AKI) This condition develops suddenly, often due to infections, dehydration, certain medications, or severe illness. In many cases, acute kidney injury can be treated and reversed if the underlying cause is identified and treated early. 2. Chronic Kidney Disease (CKD) Chronic kidney disease develops gradually over months or years. It occurs when the kidneys become permanently damaged and cannot function normally. CKD usually requires long-term management rather than a complete cure, especially in advanced stages. Can Kidney Disease Be Completely Cured? Whether kidney disease can be cured depends on the severity and type of the condition. Early-stage kidney disease may sometimes be reversed or controlled with proper medical treatment and lifestyle changes. If detected early, doctors may be able to slow or stop the progression of kidney damage. However, chronic kidney disease in advanced stages cannot be completely cured because the kidney tissue that has already been damaged cannot regenerate. In such cases, treatment focuses on controlling symptoms, preventing further damage, and improving the patient’s quality of life. For patients with severe kidney failure, treatments like dialysis or kidney transplantation may be required. Common Causes of Kidney Disease Several health conditions can lead to kidney damage. Some of the most common causes include: Diabetes High blood sugar levels can damage the blood vessels in the kidneys, reducing their ability to filter waste. High Blood Pressure Uncontrolled blood pressure can weaken the tiny filtering units in the kidneys, leading to long-term damage. Kidney Infections Repeated infections can harm kidney tissues and affect their functioning. Kidney Stones Large or untreated kidney stones may block urine flow and cause kidney damage. Autoimmune Disorders Certain immune system disorders can attack the kidneys and cause inflammation. Genetic Conditions Some inherited diseases may affect kidney function over time. Understanding these causes is important because treating the underlying problem can help protect kidney health. Early Signs and Symptoms of Kidney Disease Kidney disease often develops silently in the early stages, which is why regular health checkups are important. As the condition progresses, patients may notice symptoms such as: Swelling in the legs, ankles, or face Frequent urination, especially at night Fatigue and weakness Loss of appetite Nausea or vomiting Difficulty concentrating High blood pressure Changes in urine color or quantity If you experience these symptoms, it is important to consult a doctor for proper diagnosis and treatment. How Kidney Disease Is Diagnosed Doctors use several tests to detect kidney disease and evaluate kidney function. These tests may include: Urine Tests To check for protein, blood, or other abnormalities. Imaging Tests Ultrasound or CT scans help detect structural problems in the kidneys. Kidney Biopsy In some cases, a small sample of kidney tissue may be examined to determine the cause of damage. Early diagnosis helps doctors start treatment before the condition worsens. Treatment Options for Kidney Disease Although kidney disease cannot always be cured, proper treatment can slow its progression and help patients live healthier lives. Medications Doctors may prescribe medicines to control blood pressure, manage diabetes, reduce inflammation, and protect kidney function. Lifestyle Changes Healthy lifestyle habits can play a major role in preventing further kidney damage. Dialysis If the kidneys stop functioning properly, dialysis helps remove waste and excess fluids from the body. Kidney Transplant In severe cases of kidney failure, a kidney transplant may be recommended. This procedure replaces the damaged kidney with a healthy one from a donor. Each treatment plan is personalized depending on the patient’s condition. Can Lifestyle Changes Improve Kidney Health? Yes, lifestyle changes can significantly improve kidney health and slow the progression of kidney disease. Some important steps include: Maintaining Healthy Blood Sugar Levels People with diabetes should monitor and control their blood sugar regularly.Always warm up for 5–10 minutes before starting physical activity. This prepares your muscles for movement and reduces stiffness. Controlling Blood Pressure Keeping blood pressure within a normal range protects kidney function. Eating a Kidney-Friendly Diet Reducing salt, processed foods, and excessive protein intake can help support kidney health. Stay Hydrated Drinking enough water helps the kidneys flush out toxins effectively. Avoiding Smoking and Excess Alcohol These habits can worsen kidney damage and increase the risk of complications. Regular Exercise Physical activity helps maintain overall health and supports kidney function. Small lifestyle changes can make a big difference in protecting your kidneys. Tips to Prevent Kidney Disease Prevention is always better than treatment. You can reduce the risk of kidney disease by following these simple tips: Get regular health checkups Control diabetes and blood pressure Maintain a healthy weight Stay physically active Drink adequate water Avoid unnecessary medications or painkillers Follow a balanced and nutritious diet Taking care of your kidneys today can prevent serious health issues in the future. Frequently Asked Questions (FAQs) Can kidney disease be cured completely? In some cases, early kidney problems can be treated and reversed if detected in time. However, chronic kidney disease usually cannot be completely cured, but
Muscle Stiffness: Causes, Symptoms, Treatment & How to Reduce It Naturally
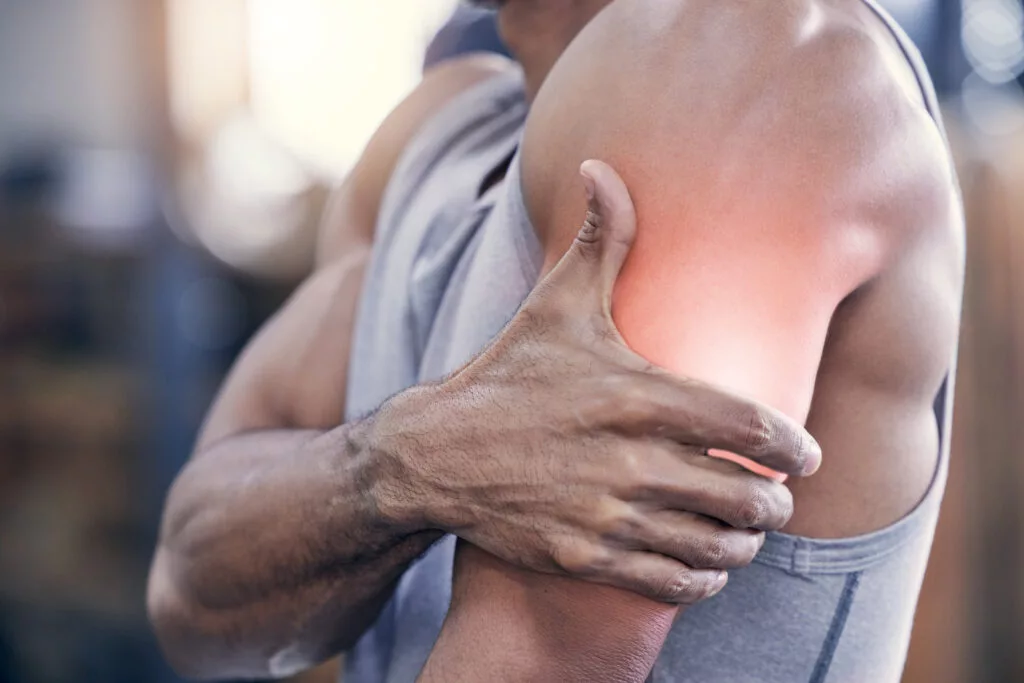
Muscle Stiffness: Causes, Symptoms, Treatment & How to Reduce It Naturally Home / Muscle stiffness is a common problem that affects people of all ages. Whether you are an athlete, a working professional sitting for long hours, or someone recovering from an injury, you may experience tight and uncomfortable muscles at some point. Understanding what is muscle stiffness, its causes, and the right muscle stiffness treatment can help you recover faster and prevent future problems. What is Muscle Stiffness? If you are wondering what is muscle stiffness, it refers to a feeling of tightness, hardness, or reduced flexibility in the muscles. When muscles become stiff, they do not move easily, and you may feel discomfort while performing regular activities such as walking, bending, or lifting objects. Muscle stiffness can occur suddenly after physical activity or gradually due to poor posture, stress, or certain medical conditions. In most cases, it is temporary and improves with rest and proper care. However, persistent muscle stiffness may require medical evaluation. Muscle Stiffness Causes There are several muscle stiffness causes, and identifying the exact reason is important for proper treatment. 1. Overuse or Intense Exercise One of the most common muscle stiffness causes is overuse. After heavy workouts or sudden physical activity, small muscle fibers may develop minor tears, leading to soreness and stiffness. This is often known as delayed onset muscle soreness (DOMS). 2. Poor Posture Sitting for long hours in front of a computer or looking down at a phone can cause stiffness in the neck, shoulders, and lower back. Poor posture keeps certain muscles contracted for long periods, leading to tightness. 3. Muscle Strain or Injury A strain, sprain, or minor muscle injury can result in pain and stiffness. In such cases, movement becomes limited due to inflammation. 4. Dehydration Muscles require proper hydration and electrolytes to function well. Dehydration can increase the risk of cramps and stiffness. 5. Stress and Anxiety When you are stressed, your body tends to tighten muscles unconsciously. Chronic stress may result in persistent muscle stiffness, especially in the neck and shoulders. 6. Medical Conditions Certain health conditions can also be responsible for muscle stiffness. These include: Fibromyalgia Parkinson’s disease Multiple sclerosis Rheumatoid arthritis If muscle stiffness is severe, long-lasting, or associated with other symptoms like weakness or tremors, medical consultation is necessary. Symptoms of Muscle Stiffness Muscle stiffness may present with the following symptoms: Tight or hard feeling in muscles Reduced flexibility Difficulty moving joints Pain while stretching Mild swelling Muscle fatigue In some cases, stiffness may also be accompanied by muscle spasms or cramps. Muscle Stiffness Treatment The right muscle stiffness treatment depends on the underlying cause. Most mild cases improve with simple home remedies, but chronic stiffness may require professional care. 1. Rest and Activity Modification Avoid activities that worsen the stiffness. Giving your muscles time to recover is essential. 2. Stretching and Mobility Exercises Gentle stretching improves flexibility and increases blood circulation. Regular stretching is one of the most effective ways to manage muscle stiffness. 3. Hot and Cold Therapy Ice packs help reduce inflammation in acute injuries. Heat therapy relaxes tight muscles and improves blood flow. Using heat before activity and ice after strain can be beneficial. 4. Massage Therapy Massage helps relieve muscle tension and enhances circulation, making it an effective muscle stiffness treatment. 5. Hydration and Proper Nutrition Drinking enough water and consuming foods rich in magnesium and potassium supports muscle health. 6. Pain Relief Medications Over-the-counter anti-inflammatory medicines may help in reducing pain and stiffness. However, they should be taken only under medical supervision. 7. Physiotherapy If stiffness persists, physiotherapy is highly recommended. A trained physiotherapist can design a customized exercise plan to improve strength, flexibility, and posture. How to Reduce Muscle Stiffness Naturally If you are searching for how to reduce muscle stiffness, here are some practical and effective tips: Warm-Up Before Exercise Always warm up for 5–10 minutes before starting physical activity. This prepares your muscles for movement and reduces stiffness. Stretch Daily Daily stretching improves flexibility and prevents tightness. Focus especially on commonly stiff areas like the neck, back, and hamstrings. Maintain Good Posture Keep your back straight and shoulders relaxed while sitting. Use ergonomic chairs if possible. Stay Hydrated Drink at least 7–8 glasses of water daily. Proper hydration helps muscles function efficiently. Take Regular Breaks If you work at a desk, take short walking breaks every 30–60 minutes to prevent muscle stiffness. Practice Yoga or Light Exercise Yoga, walking, and light strength training improve muscle flexibility and overall body balance. Get Adequate Sleep Sleep allows muscles to repair and recover. Poor sleep may worsen stiffness and fatigue. By following these habits regularly, you can significantly reduce the chances of recurring muscle stiffness. When to See a Doctor While muscle stiffness is usually harmless, you should consult a doctor if: Stiffness lasts more than two weeks There is severe pain You experience muscle weakness There is swelling, redness, or fever Stiffness affects your daily routine Early diagnosis ensures proper muscle stiffness treatment and prevents complications. Frequently Asked Questions (FAQs) What is muscle stiffness? Muscle stiffness is a condition where muscles feel tight, hard, and difficult to move, often causing discomfort and reduced flexibility. What are the main muscle stiffness causes? Common muscle stiffness causes include overuse, poor posture, dehydration, injury, stress, and certain medical conditions. How long does muscle stiffness last? Mild muscle stiffness usually improves within a few days. However, chronic stiffness may last longer and require medical evaluation. What is the best muscle stiffness treatment? The best muscle stiffness treatment depends on the cause but often includes rest, stretching, heat therapy, hydration, and physiotherapy. How to reduce muscle stiffness quickly? To reduce muscle stiffness quickly, apply heat, perform gentle stretching, stay hydrated, and take light movement breaks. Can dehydration cause muscle stiffness? Yes, dehydration can lead to muscle cramps and stiffness because muscles need proper hydration to function properly. Conclusion Muscle stiffness is a common yet manageable condition. Now
Bone Tuberculosis: Causes, Symptoms, Diagnosis & Treatment
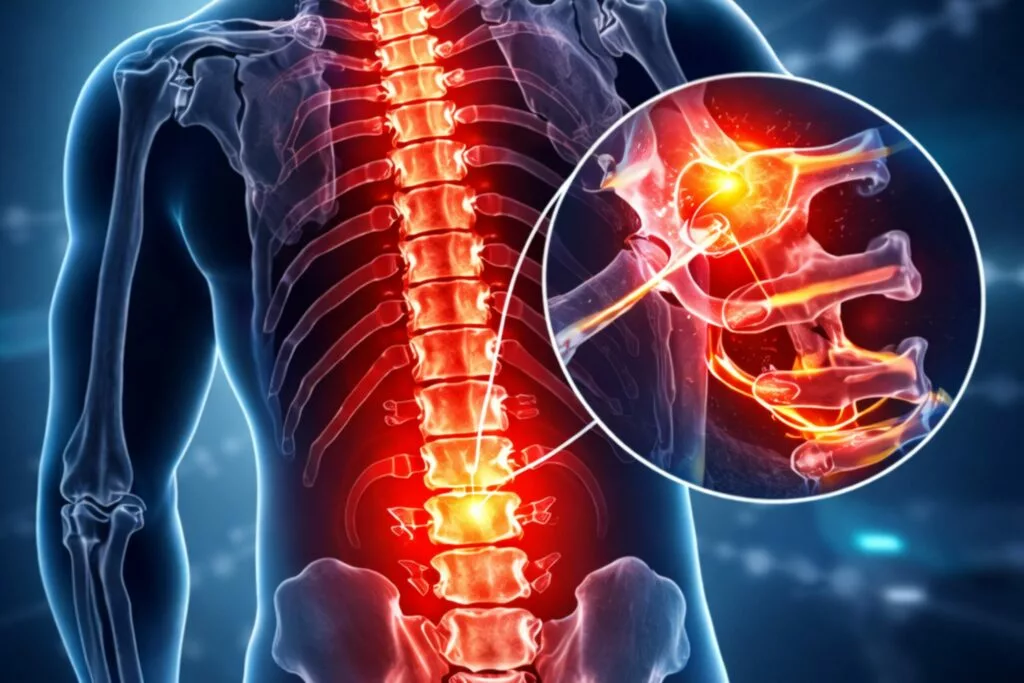
Bone Tuberculosis: Causes, Symptoms, Diagnosis & Treatment Home / Bone tuberculosis is a serious form of extrapulmonary tuberculosis that affects the bones and joints rather than the lungs. Although tuberculosis is commonly associated with pulmonary infection, skeletal involvement can lead to long-term complications if not diagnosed and treated early. In India and other developing countries, the burden of bone tuberculosis remains clinically significant, particularly in individuals with weakened immunity. This comprehensive guide explains the causes, risk factors, clinical presentation, diagnostic pathway, and modern bone tuberculosis treatment options in a structured, evidence-based manner. What Is Bone Tuberculosis? Bone tuberculosis is a chronic bacterial infection caused by Mycobacterium tuberculosis that spreads from the lungs or other primary sites to the skeletal system through the bloodstream. It most commonly affects the spine, hips, knees, and long bones. The condition is also known as: Skeletal tuberculosis Osteoarticular tuberculosis Tubercular osteomyelitis When the spine is involved, it is referred to as Spinal tuberculosis, historically called Pott’s disease. When joints are affected, it is termed Joint tuberculosis. Causes of Bone Tuberculosis Bone tuberculosis occurs when tuberculosis bacteria disseminate hematogenously from a primary focus, usually pulmonary TB. In some cases, the primary infection may be latent or asymptomatic. Main Causes Spread from active pulmonary TB Reactivation of latent TB infection Weakened immune system Poor nutrition Chronic illnesses such as diabetes HIV infection Individuals living in TB-endemic regions are at higher risk. Types of Bone Tuberculosis 1. Spinal Tuberculosis Spinal tuberculosis accounts for nearly 50% of skeletal TB cases. It commonly affects the thoracic and lumbar vertebrae. Clinical features include: Persistent back pain Spinal stiffness Vertebral collapse Kyphotic deformity Neurological deficits in advanced cases If untreated, spinal tuberculosis may cause spinal cord compression. 2. Joint Tuberculosis Joint tuberculosis typically affects weight-bearing joints such as: Hip joint Knee joint Ankle Shoulder This form presents as chronic monoarthritis with gradual joint destruction. Bone Tuberculosis Symptoms and Treatment Overview Understanding bone tuberculosis symptoms and treatment options early can significantly improve prognosis. Common Symptoms Bone tuberculosis symptoms develop gradually and may include: Persistent bone pain Swelling around joints Reduced range of motion Low-grade fever Night sweats Weight loss Fatigue In spinal tuberculosis: Back pain worsening over time Numbness or weakness in limbs Difficulty walking Because symptoms are slow and nonspecific, diagnosis is often delayed. Avoid activities that worsen the stiffness. Giving your muscles time to recover is essential. Is Bone Tuberculosis Communicable? A common concern among patients is: is bone tuberculosis communicable? Bone tuberculosis itself is not directly contagious through casual contact. However, if the individual also has active pulmonary TB, the lung infection can be transmissible via respiratory droplets. Therefore: Skeletal TB alone is generally not communicable. Active lung TB with bone involvement may pose transmission risk. Early diagnosis and complete treatment significantly reduce infectivity. Diagnosis of Bone Tuberculosis Timely diagnosis is critical to prevent irreversible bone damage. Clinical Examination Orthopedic evaluation focuses on: Local tenderness Swelling Restricted joint movement Neurological assessment in spinal casesTimely diagnosis is critical to prevent irreversible bone damage. Imaging Studies X-ray – shows bone erosion and joint narrowing MRI – gold standard for spinal tuberculosis CT scan – evaluates bone destruction Ultrasound – detects abscess formation Laboratory Tests ESR and CRP levels Tuberculin skin test (Mantoux) Interferon-gamma release assays GeneXpert test Biopsy for definitive diagnosis Biopsy remains the confirmatory test for bone tuberculosis. Bone Tuberculosis Treatment Bone tuberculosis treatment primarily involves long-term anti-tubercular therapy (ATT). Early initiation improves outcomes and reduces complications. 1. Medical Management Standard bone tuberculosis treatment includes: Isoniazid Rifampicin Pyrazinamide Ethambutol Treatment duration: Typically 9 to 12 months In spinal tuberculosis, may extend up to 18 months Compliance is essential to prevent drug resistance. 2. Surgical Management Surgery is indicated when: Neurological deficits are present Severe spinal deformity Large abscess formation Joint destruction Procedures may include: Abscess drainage Debridement Spinal stabilization Joint reconstruction Not all cases require surgery; most respond to medical therapy alone. Recovery Timeline Recovery from bone tuberculosis depends on: Severity of infection Location (spine vs joint) Timely initiation of treatment Patient immunity Typical Recovery Phases: Pain reduction: 4–6 weeks Infection control: 3–6 months Complete healing: 9–12 months Physiotherapy plays a vital role in restoring joint mobility. Complications of Untreated Bone Tuberculosis Delayed or inadequate treatment may result in: Permanent joint stiffness Limb shortening Chronic sinus formation Vertebral collapse Paralysis in spinal tuberculosis Severe deformity Early bone tuberculosis treatment prevents these outcomes. Prevention of Bone Tuberculosis Preventive strategies include: Early treatment of pulmonary TB BCG vaccination Improved nutrition Screening in high-risk populations Regular medical follow-up Key Differences – Bone TB vs Arthritis Feature Bone Tuberculosis Arthritis Cause Bacterial infection Autoimmune or degenerative Fever Common Rare Weight loss Present Absent Duration Gradual Variable Treatment Anti-TB drugs Anti-inflammatory drugs Proper diagnosis prevents mismanagement. Preventive strategies include: Early treatment of pulmonary TB BCG vaccination Improved nutrition Screening in high-risk populations Regular medical follow-up Frequently Asked Questions (FAQs) What is bone tuberculosis? Bone tuberculosis is a bacterial infection of the bones or joints caused by Mycobacterium tuberculosis spreading from another body site. What are the early bone tuberculosis symptoms? Early symptoms include persistent bone pain, swelling, mild fever, night sweats, and reduced joint movement. Is bone tuberculosis communicable? Bone tuberculosis alone is usually not communicable. However, if associated with active pulmonary TB, transmission is possible. How long does bone tuberculosis treatment take? Treatment generally lasts 9–12 months and may extend longer in spinal tuberculosis cases. Can bone tuberculosis be cured completely? Yes, with proper medical therapy and adherence to anti-tubercular drugs, bone tuberculosis can be cured completely. Is surgery necessary for bone tuberculosis? Most cases respond to medication. Surgery is reserved for complications like deformity or nerve compression. Conclusion Bone tuberculosis is a chronic but treatable infectious condition affecting the skeletal system. Early recognition of bone tuberculosis symptoms and treatment initiation are crucial to prevent long-term disability. With modern diagnostic tools and prolonged anti-tubercular therapy, outcomes are significantly improved. Awareness, timely intervention, and adherence to
Interventional Cardiology: Procedures, Conditions & Benefits
Interventional Cardiology: Procedures, Conditions Treated & Benefits Home / Interventional cardiology is a specialized branch of cardiology that focuses on diagnosing and treating heart and blood vessel conditions using minimally invasive, catheter-based procedures. These modern & advanced techniques help restore blood flow, improve heart function, and reduce the need for open-heart cardiology surgery. People looking for interventional cardiology often want to understand what it involves, which heart conditions are treated, how procedures are performed, and what benefits interventional cardiology offers compared to traditional cardiac surgery. With modern advanced imaging and precision tools, interventional cardiology has transformed the treatment of many cardiovascular diseases. This detailed guide explains what interventional cardiology is, the types of procedures performed, conditions treated, benefits, recovery expectations, and answers common patient questions in a clear and easy-to-understand way. What Is Interventional Cardiology Interventional cardiology is a subspecialty of cardiology that uses catheter-based techniques to diagnose and treat heart conditions without open surgery. Interventional cardiology focuses on: Treating blocked or narrowed heart arteries Managing structural heart diseases Improving blood flow using minimally invasive methods These procedures are typically performed through small punctures in the wrist or groin. What Does an Interventional Cardiologist Do? An interventional cardiologist specializes in diagnosing and treating heart conditions using minimally invasive procedures rather than open surgery. Their role includes: Performing angiography and stenting to diagnose and treat blocked heart arteries. Treating blocked or narrowed arteries to restore normal blood flow. Managing structural heart conditions such as valve disorders or congenital defects. Monitoring heart recovery after procedures to ensure long-term success and stability. Interventional cardiologists play an essential role in modern heart care by combining precision treatment with faster recovery. Types of Interventional Cardiology There are different types of interventional cardiology approaches based on the heart condition being treated. Common types include: Coronary interventional cardiology – Focuses on blocked heart arteries Structural heart interventions – Treats valve and heart structure problems Peripheral vascular interventions – Address blood vessel disease outside the heart Each type of interventional cardiology aims to restore heart function safely and effectively. Interventional Cardiology Procedures Interventional cardiology procedures use advanced imaging guidance and specialized catheters to diagnose and treat heart disease in a minimally invasive way, without the need for open-heart surgery. Common interventional cardiology procedures include: Coronary angiography – A diagnostic procedure used to visualize blocked or narrowed heart arteries. Angioplasty – A balloon-based technique that opens narrowed coronary arteries and improves blood flow. Stent placement – A small mesh tube is placed in an artery to keep it open after angioplasty. Balloon valvuloplasty – A procedure to widen narrowed heart valves and improve valve function. Closure of heart defects – Minimally invasive closure of abnormal openings in the heart using catheter-based devices. These interventional cardiology procedures help relieve symptoms, restore blood flow, and avoid large surgical incisions, leading to faster recovery. Conditions Treated Under Interventional Cardiology Interventional cardiology is used to treat a wide range of heart and vascular conditions that affect blood flow, heart function, and overall cardiovascular health. Conditions commonly treated include: Coronary artery disease – Narrowed or blocked heart arteries that reduce blood flow and cause chest pain or heart attacks. Heart valve disorders – Conditions where heart valves do not open or close properly, affecting blood circulation. Congenital heart defects – Structural heart problems present from birth that can be corrected using catheter-based techniques. Peripheral artery disease – Narrowing of blood vessels outside the heart that affects circulation. Certain rhythm-related heart conditions – Selected rhythm issues associated with structural or vascular abnormalities. Early interventional cardiology treatment often improves outcomes, restores blood flow, and prevents serious complications. Why You May Need Interventional Cardiology You may need interventional cardiology when heart symptoms are caused by blocked arteries or structural heart problems requiring targeted treatment. Interventional cardiology may be recommended for: Chest pain or shortness of breath is caused by reduced blood flow to the heart muscle. Recurrent heart-related symptoms that persist despite medical treatment. Reduced blood flow to the heart, increasing the risk of heart damage or heart attack. High risk of heart attack due to significant artery blockages or advanced heart disease. Early interventional cardiology treatment improves heart function and supports better long-term outcomes. Benefits of Interventional Cardiology The benefits of interventional cardiology extend beyond effective treatment by offering safer, faster, and more patient-friendly solutions for heart disease. Key benefits include: Minimally invasive procedures – Treatments are performed through small access points rather than large surgical cuts. Reduced surgical trauma – Less damage to surrounding tissues compared to open-heart surgery. Faster recovery time – Many patients return to normal activities sooner. Lower risk of complications – Reduced risk of infection and bleeding. Shorter hospital stay – Patients often require less time in the hospital after treatment. These benefits make interventional cardiology a preferred option for many heart conditions. Interventional Cardiology Uses Interventional cardiology is widely used in both emergency and planned heart care to manage complex cardiovascular conditions effectively. Common uses include: Emergency treatment of heart attacks Management of blocked heart arteries Treatment of valve-related heart diseases Alternative to open-heart surgery in selected cases The role of interventional cardiology continues to expand with advancing cardiac technology and treatment techniques. Recovery After Interventional Cardiology Recovery after interventional cardiology procedures is generally quicker and smoother compared to traditional heart surgery due to the minimally invasive nature of the treatments. Recovery factors include: Type of procedure performed – Simpler procedures often allow faster recovery. Severity of heart disease – Advanced conditions may require longer monitoring and care. Overall health of the patient – Good general health supports quicker healing. Post-procedure care and lifestyle changes – Proper follow-up, medications, and heart-healthy habits aid recovery. Many patients resume normal daily activities within days to weeks after interventional cardiology procedures. When to Seek Medical Help Early evaluation is important when heart-related symptoms appear, as delayed treatment can affect outcomes in interventional cardiology. Seek medical help if you experience: Constant chest pain that does not improve with rest or medication. Shortness of
Paediatric Pulse Oximeter Explained: Uses, Accuracy & Benefits Guide

Paediatric Pulse Oximeter Explained: Uses, Accuracy & Benefits Guide Home / A Paediatric Pulse Oximeter is a specialized, advanced medical device used to measure oxygen saturation (SpO₂) and pulse rate in infants and children. Parents and healthcare providers often search for a Paediatric Pulse Oximeter to understand how it works, how accurate it is, and when oxygen levels require medical attention. Unlike adult devices, a Paediatric Pulse Oximeter is specifically designed for smaller fingers and pediatric circulation patterns. It provides more reliable readings in children, especially during respiratory infections, asthma episodes, or post-surgical recovery. This guide explains what a Paediatric Pulse Oximeter is, its types, uses of Paediatric Pulse Oximeter, functions, accuracy, benefits, and when to see a doctor for abnormal readings. What is a Paediatric Pulse Oximeter? A Paediatric Pulse Oximeter is a non-invasive medical device used to measure oxygen saturation (SpO₂) and pulse rate in infants and children safely and quickly. It measures: Oxygen saturation (SpO₂) – Indicates the level of oxygen in the blood Pulse rate – Measures heart rate Peripheral perfusion – Assesses blood circulation quality A Paediatric Pulse Oximeter uses light sensors on a child’s finger or toe to measure oxygen levels in real time. It is designed for smaller digits, ensuring more accurate, child-specific readings than adult devices. Types of Paediatric Pulse Oximeter Different Types of Paediatric Pulse Oximeter are designed based on age group and clinical requirements. 1. Fingertip Paediatric Pulse Oximeter This type of Paediatric Pulse Oximeter is commonly used for older children and home monitoring. Compact and portable Easy to use Suitable for mild respiratory monitoring 2. Handheld Paediatric Pulse Oximeter A handheld Paediatric Pulse Oximeter is typically used in hospitals and clinics for more detailed monitoring. Higher clinical accuracy Suitable for neonates and infants Allows continuous assessment 3. Wrap-around or Sensor-Based Devices These Types of Paediatric Pulse Oximeter are designed for newborns and critical care settings. Ideal for newborns Enables continuous monitoring Frequently used in NICU environments Choosing the right Types of Paediatric Pulse Oximeter depends on the child’s age, medical condition, and how frequently oxygen monitoring is required. Uses of Paediatric Pulse Oximeter The uses of the Paediatric Pulse Oximeter extend across preventive, diagnostic, and emergency settings. A Paediatric Pulse Oximeter is commonly used for: Monitoring asthma and bronchitis Detecting pneumonia-related oxygen drop Managing congenital heart disease Monitoring post-surgical recovery Evaluating sleep apnea in children COVID-19 and viral respiratory monitoring Parents often use a Paediatric Pulse Oximeter at home to ensure early detection of oxygen desaturation. Functions of Paediatric Pulse Oximeter The primary functions of a Paediatric Pulse Oximeter focus on monitoring a child’s oxygen levels and heart rate safely and accurately. Key functions include: Measuring blood oxygen saturation (SpO₂) Displaying pulse rate Showing perfusion index (in advanced models) Alerting to abnormal readings A modern Paediatric Pulse Oximeter may also include low-oxygen alarms and a clear digital display, helping caregivers respond quickly. The primary functions of a Paediatric Pulse Oximeter focus on monitoring a child’s oxygen levels and heart rate safely and accurately. Accuracy of Paediatric Pulse Oximeter The accuracy of a Paediatric Pulse Oximeter depends on correct use and device quality. When used properly, it provides reliable SpO₂ and pulse rate readings in children. Factors That Ensure Better Accuracy: Proper sensor placement on the finger or toe The child remains still during measurement Warm extremities for good blood flow Use of a high-quality, clinical-grade device Clinical-grade Paediatric Pulse Oximeter devices typically offer an accuracy range of ±2% for SpO₂ readings. Factors That May Affect Accuracy: Cold hands or poor circulation Nail polish or artificial nails Excess movement Incorrect probe size For consistent and reliable readings, always use an appropriately sized Paediatric Pulse Oximeter designed specifically for children. Results from Paediatric Pulse Oximeter Understanding results from the Paediatric Pulse Oximeter is important. Normal Range of Oxygen in Children: 95%–100% SpO₂ is considered normal If readings drop below 94%, medical consultation may be required. Benefits of Paediatric Pulse Oximeter The Benefits of Paediatric Pulse Oximeter make it an important monitoring tool in both hospital and home settings. A Paediatric Pulse Oximeter allows safe and continuous observation of oxygen levels in children with respiratory or cardiac concerns. Key benefits include: Early detection of hypoxia Non-invasive and painless monitoring Quick results within seconds Home-based safety monitoring Reduced emergency risk Improved chronic disease management Because of these Paediatric Pulse Oximeter benefits, it is widely recommended for children with asthma, pneumonia, congenital heart disease, and other respiratory conditions requiring regular oxygen monitoring. When to See a Doctor While a Paediatric Pulse Oximeter is useful for monitoring oxygen levels at home, medical evaluation is necessary if abnormal readings or symptoms appear. You should consult a pediatric specialist if: Oxygen saturation levels drop below 94% The child shows rapid or labored breathing Bluish lips or nail beds are noticed A constant cough is associated with low oxygen levels Repeated abnormal results from the Paediatric Pulse Oximeter Although a Paediatric Pulse Oximeter helps detect early oxygen changes, it should not replace professional diagnosis or emergency care when serious symptoms are present. How to Use a Paediatric Pulse Oximeter Parents frequently ask, How to use a pediatric pulse oximeter correctly? Proper technique improves the reliability of readings from a Paediatric Pulse Oximeter. Steps to Follow: Ensure the child’s hand or foot is warm. Place the Paediatric Pulse Oximeter securely on a finger or toe. Keep the child calm and still. Wait 10–20 seconds for a stable SpO₂ and pulse reading. Record the oxygen saturation and pulse rate for tracking. Regular and correct use of a Paediatric Pulse Oximeter ensures accurate monitoring of a child’s respiratory health. Why Pulse Oximetry Should Be Monitored in Pediatric Patients Pulse oximetry is critical in pediatric care because children deteriorate faster than adults during respiratory distress. Monitoring with a Paediatric Pulse Oximeter helps: Detect silent hypoxia Monitor acute infections Prevent emergency complications Support safe home monitoring FAQs on Paediatric Pulse Oximeter What is a pediatric pulse oximeter? A Paediatric Pulse
Orthopedic Disability: Causes, Types, Assessment & Treatment Guide

Orthopedic Disability: Causes, Types, Assessment & Treatment Guide Home / Orthopedic disability refers to physical impairment affecting bones, joints, muscles, ligaments, or nerves that limits movement and functional ability. People searching for orthopedic disability often want to understand what orthopedic disability is, what causes it, how it is assessed, and what treatment options are available. An orthopedic disability may result from injury, congenital conditions, degenerative joint disease, spinal disorders, or trauma. Early diagnosis and structured management can significantly improve mobility, independence, and quality of life. This comprehensive guide explains what orthopedic disability is, the types of orthopedic disability, causes of orthopedic disability, symptoms, assessment methods, orthopedic disability treatment options, prevention strategies, and when to see a doctor. What is Orthopedic Disability? To understand what orthopedic disability is, it is important to know that it involves a physical impairment of the musculoskeletal system that restricts normal movement, coordination, or posture. Orthopedic disability may affect: Bones and joints Muscles and tendons Ligaments Spine and spinal alignment Limbs and weight-bearing structures An orthopedic disability can be temporary or permanent, mild or severe, and may significantly impact daily functional activities such as walking, standing, lifting, or performing self-care tasks. Types of Orthopedic Disability The types of orthopedic disability vary depending on the cause, affected structure, and severity 1. Congenital Orthopedic Disability This type of orthopedic disability is present from birth and develops due to abnormal musculoskeletal formation. Common examples include: Clubfoot – Abnormal positioning of the foot at birth Limb deformities – Structural abnormalities affecting arms or legs Developmental hip dysplasia – Improper hip joint formation Early diagnosis and corrective treatment can reduce long-term orthopedic disability. 2. Acquired Orthopedic Disability Acquired orthopedic disability develops after birth due to injury, trauma, or disease. Examples include: Fracture-related deformities – Improper healing of broken bones Post-traumatic joint stiffness – Restricted joint movement after injury Spinal injuries – Trauma affecting spinal stability and mobility Timely orthopedic care can prevent progression to permanent orthopedic disability. 3. Degenerative Orthopedic Disability Degenerative orthopedic disability occurs due to the gradual wear and tear of joints and cartilage. Common conditions include: Osteoarthritis Rheumatoid arthritis Severe joint degeneration Chronic inflammation and cartilage loss often lead to long-term orthopedic disability if untreated. 4. Neuromuscular-Related Orthopedic Disability his form of orthopedic disability results from neurological or muscular disorders affecting movement. Examples include: Cerebral palsy Muscular dystrophy Post-stroke limb weakness Identifying the correct type of orthopedic disability ensures targeted medical management and rehabilitation planning. Causes of Orthopedic Disability The causes of orthopedic disability may be congenital, traumatic, degenerative, infectious, or inflammatory in nature. Identifying the root cause is crucial for effective prevention and treatment. Common causes of orthopedic disability include: Road traffic accidents Sports injuries Severe fractures Chronic arthritis Spinal cord injuries Bone infections Genetic disorders Long-standing inflammation, untreated joint disease, or delayed orthopedic intervention can gradually result in permanent orthopedic disability. Early medical evaluation significantly reduces complications. Symptoms of Orthopedic Disability The symptoms of orthopedic disability depend on the specific joint, bone, or muscle involved. These symptoms may develop gradually or suddenly after trauma. Common symptoms include: Difficulty walking or bearing weight Joint stiffness, especially after rest Limb deformity or abnormal posture Constant musculoskeletal pain Muscle weakness affecting daily tasks Reduced range of motion Balance problems and instability In severe cases, orthopedic disability may cause dependence on mobility aids such as crutches, braces, or wheelchairs. Assessment of Orthopedic Disability Accurate assessment of orthopedic disability is essential for treatment planning and disability certification (if required). Assessment typically includes: Detailed medical history Physical examination Range of motion testing Muscle strength evaluation X-rays and imaging studies Functional ability scoring In India, disability percentage may be calculated using standardized medical guidelines for orthopedic disability assessment. Early evaluation improves long-term outcomes and rehabilitation success. Treatment of Orthopedic Disability The treatment of orthopedic disability depends on the severity of functional limitation, the affected joint or bone, and the underlying pathology. Early and structured management plays an important role in improving mobility and quality of life. Non-Surgical Treatment Non-surgical treatment of orthopedic disability is often recommended in mild to moderate cases and focuses on restoring strength and function. It may include: Orthopedic Physiotherapy to improve joint mobility Strengthening exercises for muscle support Bracing support for joint stabilization Pain management through medications Occupational therapy for daily activity training Assistive devices such as walkers or orthotic supports Surgical Treatment Surgical treatment of orthopedic disability is considered when conservative methods fail or structural correction is required. Common procedures include: Fracture correction surgery Joint replacement surgery Tendon reconstruction Spinal surgery Corrective osteotomy Timely treatment of orthopedic disability can significantly restore movement, reduce deformity, and improve long-term independence. Prevention of Orthopedic Disability Prevention of orthopedic disability focuses on early identification of musculoskeletal problems and proper injury management. Proactive care helps reduce the risk of long-term joint damage and mobility issues. Preventive Measures Include: Prompt treatment of fractures and injuries Regular exercise to strengthen bones and muscles Weight management to reduce joint stress Early arthritis management Fall prevention strategies in elderly individuals Use of protective sports equipment during activities Preventing musculoskeletal injuries and addressing joint problems early greatly lowers the long-term risk of orthopedic disability. When to See a Doctor Early medical consultation and evaluation are important when symptoms begin to affect mobility or daily activities. Delaying care may increase the risk of permanent orthopedic disability. You should consult an orthopedic specialist if you experience: Constant joint pain Progressive limb deformity Difficulty walking or balancing Weakness in arms or legs Post-injury instability Sudden loss of mobility Early intervention not only reduces complications but also helps prevent the progression of orthopedic disability and long-term functional impairment. Orthopedic Disability What are the types of orthopedic disabilities? The types of orthopedic disability include congenital deformities, traumatic injuries, degenerative joint disease, and neuromuscular conditions affecting bones and joints. What are orthopedic disorders? Orthopedic disorders refer to medical conditions affecting bones, joints, ligaments, muscles, and spine that may lead to orthopedic disability if untreated. What are
Interventional Neurology: Procedures, Conditions Treated & Benefits

Interventional Neurology: Procedures, Conditions Treated & Benefits Home / Interventional neurology is a specialized branch of neurology that focuses on diagnosing and treating complex neurological conditions using minimally invasive, image-guided procedures. These techniques allow specialists to treat brain, spine, and blood vessel disorders with greater accuracy and reduced recovery time. People searching for interventional neurology often want to understand what it involves, which conditions it treats, how it differs from traditional neurology treatment, and what benefits it offers compared to open surgery. With advancements in imaging and catheter-based techniques, interventional neurology has transformed the management of many serious neurological disorders. This detailed guide explains what interventional neurology is, the types of procedures performed, conditions treated, benefits, recovery expectations, risks, and answers common patient questions in a clear and patient-friendly way. What Is Interventional Neurology Interventional neurology is a subspecialty of neurology that uses minimally invasive, catheter-based techniques to diagnose and treat disorders of the brain, spine, and nervous system. Interventional neurology focuses on: Image-guided neurological procedures Catheter-based treatment of blood vessel disorders Targeted therapy with minimal surgical exposure Unlike traditional surgery, interventional neurology procedures are usually performed through small incisions, often via blood vessels. Types of Interventional Neurology There are different types of interventional neurology approaches based on the neurological condition being treated. Common types include: Neurovascular intervention – Focuses on disorders of the brain and spinal blood vessels Endovascular neurology – Treats conditions using catheter-based vascular techniques Minimally invasive spinal interventions – Address selected spine-related neurological issues Each type of interventional neurology aims to treat conditions with precision and reduced trauma. Interventional Neurology Procedures Interventional neurology procedures are performed using modern & advanced imaging guidance and specialized instruments. Common interventional neurology procedures include: Cerebral angiography Thrombectomy for stroke Aneurysm coiling Stenting of narrowed blood vessels Embolization of abnormal vessels These procedures allow targeted treatment while minimizing damage to surrounding brain tissue. Conditions Treated Under Interventional Neurology Interventional neurology is used to treat a wide range of neurological and neurovascular conditions that affect the brain, spine, and blood vessels of the nervous system. Conditions commonly treated include: Ischemic and hemorrhagic stroke – Interventional neurology procedures help restore blood flow or control bleeding in emergency situations. Brain aneurysms – Minimally invasive techniques are used to secure weakened blood vessels and prevent rupture. Arteriovenous malformations (AVMs) – Abnormal connections between arteries and veins are treated using targeted, image-guided methods. Narrowed or blocked brain arteries – Procedures improve circulation and reduce the risk of stroke. Certain spinal vascular disorders – Selected spine-related blood vessel conditions can be managed without open surgery. Early interventional neurology treatment often improves outcomes, limits brain damage, and reduces long-term neurological disability. Benefits of Interventional Neurology The benefits of interventional neurology extend beyond treatment effectiveness by offering safer and more accurate solutions for complex neurological conditions. Key benefits include: Minimally invasive approach – Procedures are performed through small access points, avoiding large surgical incisions. Reduced surgical trauma – Less damage to surrounding tissues compared to traditional surgery. Faster recovery time – Many patients recover more quickly and resume daily activities sooner. Lower complication risk – Reduced infection and bleeding risks due to minimally invasive techniques. Shorter hospital stay – Patients often require less time in the hospital after treatment. These advantages make interventional neurology a preferred option for managing many neurological and neurovascular conditions. Interventional Neurology Uses Interventional neurology is widely used in both emergency and planned neurological care to diagnose and treat complex conditions effectively. Common uses include: Emergency stroke treatment – Rapid intervention helps minimize brain damage and improve recovery. Management of complex vascular brain disorders – Treats conditions that are difficult to manage with medication alone. Diagnosis of unexplained neurological symptoms – Advanced imaging helps identify underlying vascular problems. Alternative to open brain surgery in selected cases – Provides a less invasive treatment option for suitable patients. The use of interventional neurology continues to expand as technology advances and treatment techniques evolve. Why You May Need Interventional Neurology You may need interventional neurology when neurological symptoms are linked to blood vessel abnormalities in the brain or spine that require precise, minimally invasive treatment rather than medication alone. Interventional neurology may be recommended for: Sudden weakness or speech difficulty – Symptoms that may indicate an acute stroke requiring urgent interventional neurology care. Recurrent strokes or transient ischemic attacks – Repeated events suggesting underlying vascular problems that need targeted treatment. Known brain aneurysms – Conditions that carry a risk of rupture and may benefit from preventive interventional procedures. Progressive neurological symptoms – Worsening weakness, vision, or coordination issues linked to vascular abnormalities. Timely referral to interventional neurology improves treatment success, limits neurological damage, and supports better recovery. Recovery After Interventional Neurology Recovery after interventional neurology procedures is generally faster and smoother compared to traditional open neurological surgery due to the minimally invasive approach. Recovery factors include: Type of procedure performed – Simpler diagnostic or vascular procedures often allow quicker recovery. Severity of the neurological condition – More complex conditions may require longer monitoring and rehabilitation. Overall patient health – Good general health supports faster healing and better outcomes. Post-procedure monitoring and care – Careful observation helps prevent complications and supports safe recovery. Many patients resume normal daily activities within days to weeks after interventional neurology treatment, depending on the condition treated. When to Seek Medical Help Early consultation & evaluation is important when neurological symptoms appear, as delayed treatment can affect outcomes in many conditions managed by interventional neurology. Seek medical help if you experience: Sudden weakness or numbness – Especially on one side of the body. Severe headache or vision changes – Possible signs of bleeding or vascular issues. Difficulty speaking or understanding speech – Common warning signs of stroke. Loss of balance or coordination – May indicate brain or spinal involvement. Prompt diagnosis allows early interventional neurology treatment, improves outcomes, and reduces the risk of long-term neurological complications. FAQs on Interventional Neurology What do interventional neurologists do? Interventional neurologists diagnose and treat neurological conditions using

