Orthopedic Physiotherapy: Treatment, Benefits & When You Need It
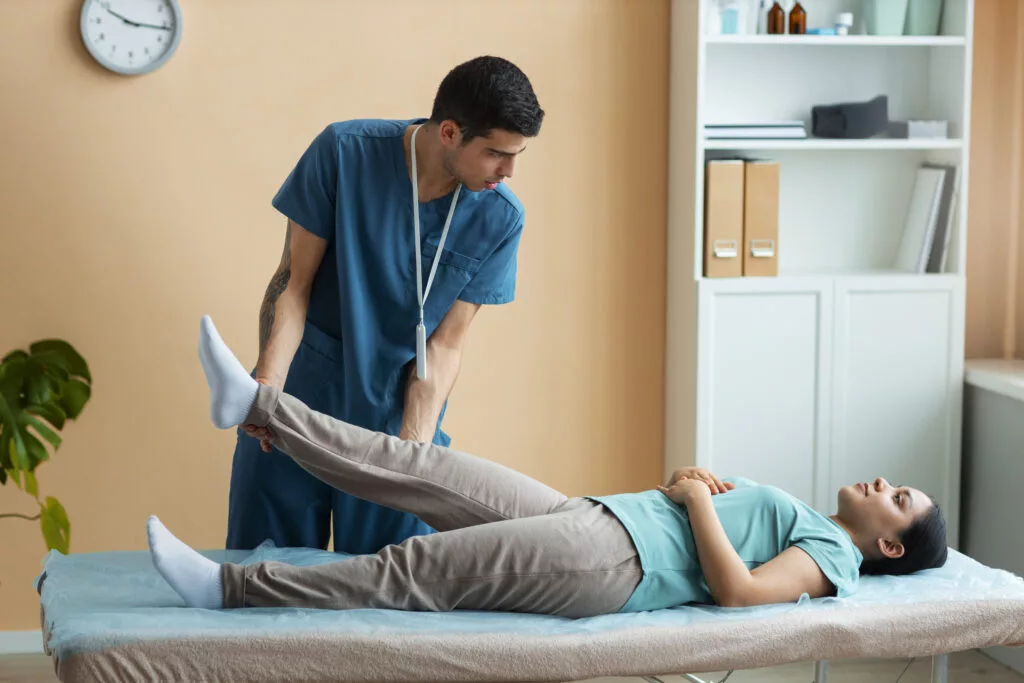
Orthopedic Physiotherapy: Treatment, Benefits & When You Need It Home / Orthopedic physiotherapy helps restore movement, reduce pain, and improve physical function in people with bone, joint, and muscle conditions. It uses non-surgical, evidence-based rehabilitation techniques for musculoskeletal problems. Orthopedic physiotherapy treatment is commonly used for joint pain, muscle stiffness, sports injuries, fractures, and post-surgical recovery. The goal is to improve mobility, strength, and daily activities while preventing long-term issues. People searching for orthopedic physiotherapy often want to know how it works, which conditions it treats, and when it is needed. Understanding this helps patients choose the right rehabilitation approach. What Is Orthopedic Physiotherapy? Orthopedic physiotherapy is a specialized branch of physiotherapy that focuses on the assessment, treatment, and rehabilitation of musculoskeletal conditions involving bones, joints, muscles, ligaments, and tendons. It is commonly used to manage pain, restore mobility, and improve function after injuries, surgeries, or chronic orthopedic conditions. Orthopedic physiotherapy is also an important part of orthopedic rehabilitation and long-term recovery planning. Orthopedic Physiotherapy Treatment Orthopedic physiotherapy treatment is designed to address pain, stiffness, weakness, and movement limitations caused by orthopedic conditions. Treatment plans are customized based on the patient’s condition, severity, and functional goals. Orthopedic physiotherapy treatment commonly includes: Pain management techniques Joint and soft tissue mobilization Muscle-strengthening exercises Stretching and flexibility training Postural correction and movement re-education The goal of orthopedic physiotherapy treatment is not only symptom relief but also long-term functional improvement. In What Conditions Is Orthopedic Physiotherapy Used? Orthopedic physiotherapy is used in a wide range of musculoskeletal conditions that affect daily activities and physical function. It is often recommended before or after surgery and as an essential part of conservative management. Common conditions treated with orthopedic physiotherapy include: Back pain, neck pain, and spine disorders Knee, hip, shoulder, and ankle pain Sports injuries and overuse injuries Fractures and post-traumatic stiffness Arthritis and degenerative joint conditions Early orthopedic physiotherapy helps prevent complications and speeds up recovery. What Does Orthopedic Physiotherapy Consist Of? Orthopedic physiotherapy consists of a structured combination of hands-on techniques and therapeutic exercises designed to restore normal activities and reduce pain. Each treatment plan is customized to the patient’s condition, severity, and recovery goals. Core components of orthopedic physiotherapy include: Therapeutic exercises to improve muscle strength, flexibility, and joint stability Manual therapy to enhance joint mobility and reduce stiffness Functional training to support daily activities and movement patterns Pain-relieving modalities when required for inflammation or discomfort Posture and injury-prevention education to avoid recurrence As recovery progresses, orthopedic physiotherapy programs are adjusted to match improving strength and mobility. Principles of Orthopedic Physiotherapy Orthopedic physiotherapy is guided by proven rehabilitation principles that ensure safe, effective, and sustainable recovery. These principles help therapists design treatments that address both symptoms and underlying movement issues. Key principles of orthopedic physiotherapy include: Individualized treatment planning based on diagnosis and functional needs Progressive loading and strengthening to rebuild muscle and joint capacity Movement correction and biomechanics to restore proper alignment Functional, goal-oriented therapy focused on daily activities Continuous reassessment and progression to support ongoing improvement By following these principles, orthopedic physiotherapy promotes long-term joint health, mobility, and independence. Benefits of Orthopedic Physiotherapy Orthopedic physiotherapy provides both immediate pain relief and long-term functional improvement for people with musculoskeletal conditions. It focuses on restoring normal movement while preventing future injuries. Major benefits include: Reduced pain and inflammation through targeted therapy Improved joint mobility and flexibility for better movement Increased muscle strength and endurance to support joints Faster recovery after injury or orthopedic surgery Better posture and movement efficiency in daily activities With consistent orthopedic physiotherapy, patients experience improved independence, mobility, and overall quality of life. How Can Orthopedic Physical Therapy Help You? Orthopedic physical therapy helps by addressing the root cause of pain rather than only managing symptoms. It focuses on restoring normal movement patterns and preventing recurrence. Orthopedic physical therapy helps you: Move with less pain Regain strength and confidence Prevent future injuries Improve daily function and activity tolerance What Conditions Does an Orthopedic Physical Therapist Treat? An orthopedic physical therapist treats a wide range of conditions involving muscles, bones, joints, and connective tissues. Treatment plans are customized based on the specific orthopedic problem. Common conditions include: Joint pain, stiffness, and reduced mobility Muscle strains, ligament injuries, and tendon problems Post-surgical rehabilitation after orthopedic procedures Sports-related injuries affecting movement and strength Chronic orthopedic conditions such as arthritis Orthopedic physiotherapy helps manage both acute injuries and long-term musculoskeletal disorders. What to Expect From an Orthopedic Physiotherapy Session An orthopedic physiotherapy session begins with a detailed assessment of pain, movement, strength, and functional limitations. During a session, you can expect: Personalized exercise programs Hands-on therapy when needed Movement and posture training Functional activity practice Progress tracking and plan adjustments Sessions are structured, safe, and goal-focused. When to See a Doctor or Orthopedic Physiotherapist Early medical or physiotherapy consultation is important when musculoskeletal symptoms begin to affect daily activities or comfort. Timely care helps prevent worsening of the condition. You should seek orthopedic physiotherapy if you experience: Constant joint or muscle pain Difficulty moving, bending, or stiffness Swelling, weakness, or pain after injury Discomfort affecting work or daily activities Slow or incomplete recovery after surgery or trauma Timely orthopedic physiotherapy improves recovery speed, movement quality, and long-term outcomes. FAQs on Orthopedic Physiotherapy What do orthopedic physios do? Orthopedic physios assess and treat musculoskeletal conditions using exercises, manual therapy, and rehabilitation techniques to restore movement and reduce pain. What is the difference between physiotherapy and orthopedic physiotherapy? Physiotherapy covers various conditions, while orthopedic physiotherapy specifically focuses on bones, joints, muscles, and orthopedic rehabilitation. What conditions require orthopedic physiotherapy? Conditions such as joint pain, sports injuries, fractures, arthritis, and post-surgical recovery commonly require orthopedic physiotherapy. What is the role of orthopedic physiotherapy? The role of orthopedic physiotherapy is to reduce pain, restore mobility, improve strength, and prevent future musculoskeletal problems. When should I see an orthopedic physiotherapist? You should see an orthopedic physiotherapist when pain, stiffness, or
Neurological Physiotherapy: Treatment, Benefits & When You Need It
Neurological Physiotherapy: Treatment, Benefits & When You Need It Home / Neurological physiotherapy plays a critical role in restoring movement, balance, and functional independence in people affected by neurological disorders and diseases. Conditions involving the brain, spinal cord, or nerves often disrupt normal motor control, strength, coordination, and sensation, making daily activities difficult. People searching for neurological physiotherapy usually want to understand how this specialized therapy works, which neurological conditions require treatment, what the recovery process looks like, and when they should seek professional help. Early evaluation & rehabilitation can significantly improve outcomes and prevent long-term disability. This detailed guide explains what neurological physiotherapy is, the conditions it treats, treatment techniques, benefits, principles, and what to expect from a neurological physiotherapy session—using clear, patient-friendly language. What Is Neurological Physiotherapy? Neurological physiotherapy is a specialized branch of physiotherapy focused on treating movement and functional problems caused by neurological disorders and diseases affecting the brain, spinal cord, and peripheral nerves. Unlike general physiotherapy, neurological physiotherapy targets impaired nerve-muscle communication, balance, posture, coordination, and motor control. Treatment plans are highly individualized, based on the type and severity of neurological involvement. Neurological physiotherapy treatment aims to restore function, improve independence, and enhance quality of life through structured rehabilitation. Neurological Disorders and Diseases Treated Neurological physiotherapy is commonly used to manage a wide range of neurological disorders and diseases that affect movement and daily function. Common Neurological Conditions Include: Stroke and post-stroke paralysis Parkinson’s disease Multiple sclerosis Spinal cord injury Traumatic brain injury Cerebral palsy Peripheral nerve injuries Motor neuron diseases Each condition presents differently, which is why neurological physiotherapy programs are tailored to individual needs. In What Conditions Is Neurological Physiotherapy Used? Neurological physiotherapy is recommended whenever a neurological condition interferes with normal movement, balance, coordination, or muscle control. These problems usually arise due to damage or dysfunction of the brain, spinal cord, or nerves, affecting a person’s ability to perform daily activities comfortably. It is commonly used in: Weakness or paralysis after a stroke, where neurological physiotherapy helps restore movement and muscle control Gait and balance problems, reducing the risk of falls, and improving walking confidence Loss of coordination or fine motor skills, affecting hand function and daily tasks Muscle stiffness, spasticity, or tremors are often seen in conditions like Parkinson’s disease Difficulty walking, standing, or performing daily activities due to impaired nerve signals Early neurological physiotherapy intervention significantly improves recovery potential, prevents secondary complications, and supports long-term functional independence. Neurological Physiotherapy Treatment Approach Neurological physiotherapy treatment focuses on retraining the nervous system by encouraging proper movement patterns through repeated, goal-oriented activities. The approach is patient-specific and depends on the type and severity of the neurological disorder. Key Components of Treatment Include: Muscle strengthening and re-education to improve controlled movement Balance and coordination training to enhance stability and posture Gait and posture correction to support safe and efficient walking Functional task training, such as sitting, standing, or grasping objects Sensory stimulation techniques to improve nerve response and awareness As neurological recovery progresses, treatment plans are adjusted to match the patient’s improving abilities, ensuring continuous improvement and safe rehabilitation. What Does Neurophysiotherapy Consist Of? Neurophysiotherapy consists of structured, evidence-based therapeutic techniques aimed at promoting neural recovery and functional improvement. These techniques are designed to stimulate the nervous system and encourage adaptive movement strategies. Core Elements Include: Task-specific movement training to restore purposeful activities Stretching and spasticity management to reduce stiffness and improve flexibility Functional electrical stimulation (when required) to activate weak muscles Breathing and endurance exercises to improve overall physical capacity Assistive device training, such as walkers or braces, for safe mobility Neurophysiotherapy is progressive in nature and adapts continuously as neurological function improves, helping patients regain independence and confidence in daily life. Principles of Neurological Physiotherapy Neurological physiotherapy is based on well-established scientific principles that focus on restoring movement, function, and independence after neurological damage. These principles guide how therapy is planned, delivered, and progressed for each patient. Key Principles Include: Neuroplasticity, which refers to the brain’s ability to reorganize and form new neural connections after injury Repetition and intensity of movement help reinforce correct movement patterns Goal-oriented functional training, focusing on real-life activities rather than isolated exercises Patient-centered goal setting, ensuring therapy aligns with individual needs and daily challenges Continuous reassessment and progression, allowing treatment to evolve with recovery Together, these principles help maximize functional recovery and long-term neurological improvement. Benefits of Neurological Physiotherapy Neurological physiotherapy provides meaningful physical, functional, and psychological benefits for individuals living with neurological disorders. With consistent therapy, patients often experience gradual but lasting improvements. Major Benefits Include: Improved mobility and balance, reducing the risk of falls Better muscle strength and coordination, supporting smoother movement Reduced stiffness and muscle tightness, improving comfort and flexibility Enhanced independence in daily activities, such as walking, dressing, or eating Improved confidence and overall quality of life, through better functional control Regular neurological physiotherapy plays an important role in long-term neurological rehabilitation and functional recovery. What to Expect From a Neurological Physiotherapy Session A neurological physiotherapy session begins with a thorough assessment to understand the patient’s movement patterns, strength, balance, and functional limitations. This helps create a personalized treatment plan. During a Session, You Can Expect: Individualized exercise programs tailored to neurological deficits Hands-on therapeutic techniques to guide and correct movement Gait and posture training for safer and more efficient mobility Functional task practice, such as standing, walking, or reaching Progress monitoring and adjustments, based on ongoing improvement Sessions are structured, safe, and adapted to the patient’s tolerance and recovery stage. When to See a Doctor or Physiotherapist Early medical evaluation is essential when neurological symptoms appear, as timely intervention improves recovery outcomes. Delaying care may lead to worsening symptoms or prolonged disability. You should seek help if you experience: Sudden weakness or paralysis in the face, arms, or legs Loss of balance or coordination, especially during walking Slurred speech or difficulty walking Tremors or muscle stiffness affecting daily activities Numbness or sensory changes that are constant or worsen Prompt referral to
Top 10 Common Gynecological Disorders: Symptoms, Causes & Treatment
Top 10 Common Gynecological Disorders: Symptoms, Causes & Treatment Home / Gynecological disorders are conditions that affect the female reproductive system and can impact menstrual health, fertility, and overall well-being. These disorders are common and can occur at any stage of a woman’s life. Many women experience various gynecological problems, such as irregular periods, pelvic pain, or abnormal discharge, but often delay medical care. Early awareness & treatment of gynecological disorders help prevent long-term complications. Understanding common gynecological disorders allows women to recognize symptoms early and seek timely treatment for better reproductive health outcomes. What Are Gynecological Disorders? Gynecological disorders refer to medical conditions that affect the female reproductive system, including the uterus, ovaries, fallopian tubes, cervix, and vagina. These conditions can impact menstrual health, fertility, pregnancy, and overall quality of life. Gynecological disorders can occur at any age—from adolescence to menopause—and may range from mild hormonal imbalances to serious conditions requiring medical or surgical treatment. Early diagnosis and timely care are important for effectively managing gynecological problems. Common Gynecological Problems in Women Gynecological problems are common and often underreported due to hesitation or lack of awareness. Many women experience symptoms but delay consultation, which can worsen the condition. Common gynecological problems include: Irregular or painful periods – caused by hormonal imbalance or underlying gynecological disorders Pelvic pain – linked to conditions like endometriosis or uterine fibroids Vaginal infections – affect vaginal health due to bacterial or fungal causes Fertility issues – related to ovulation disorders or reproductive system problems Hormonal imbalances – impacting menstrual cycles and overall gynecological health Common Symptoms of Gynecological Disorders Gynecological disorders often present with noticeable symptoms. These symptoms should not be ignored, especially if they are constant. Common symptoms include: Irregular, heavy, or painful menstrual cycles Pelvic or lower abdominal pain Abnormal vaginal discharge or odor Pain during intercourse Difficulty conceiving Abnormal bleeding between periods Constant symptoms usually indicate an underlying gynecological condition that needs evaluation. Common Causes of Gynecological Disorders Gynecological disorders develop due to a combination of medical, hormonal, and lifestyle factors. Identifying the cause helps guide accurate gynecological treatment. Common causes include: Hormonal imbalances – disrupt normal menstrual and reproductive function Infections – affecting the uterus, ovaries, or vagina Genetic or congenital conditions – impacting reproductive organ structure Poor menstrual hygiene – increases infection risk Stress and lifestyle factors – influencing hormonal health Obesity or sudden weight changes – affecting estrogen balance Top 10 Common Types of Gynecological Disorders Below are the 10 most common gynecological disorders, explained individually with symptoms and causes. 1. Polycystic Ovary Syndrome (PCOS) PCOS is a hormonal gynecological disorder that affects women of reproductive age and is a leading cause of menstrual irregularities and infertility. Common symptoms: Irregular or missed menstrual periods Excess facial or body hair growth Acne and unexplained weight gain Common causes: Hormonal imbalance involving excess androgens Insulin resistance Genetic predisposition 2. Endometriosis Endometriosis is a chronic gynecological disorder where tissue similar to the uterine lining grows outside the uterus, leading to pain and fertility issues. Common symptoms: Severe menstrual cramps Chronic pelvic pain Pain during intercourse Common causes: Retrograde menstruation Immune system dysfunction Hormonal influence 3. Uterine Fibroids Uterine fibroids are non-cancerous growths in the uterus and are among the most common gynecological problems in women. Common symptoms: Heavy or prolonged menstrual bleeding Pelvic pressure or fullness Frequent urination Common causes: Estrogen and progesterone imbalance Genetic factors Hormonal stimulation 4. Pelvic Inflammatory Disease (PID) PID is a serious gynecological disorder caused by infection of the reproductive organs, often requiring immediate medical attention. Common symptoms: Lower abdominal or pelvic pain Fever and fatigue Abnormal vaginal discharge Common causes: Untreated sexually transmitted infections Bacterial infections spreading to the uterus Delayed treatment of vaginal infections 5. Vaginal Infections Vaginal infections are frequent gynecological disorders that affect vaginal health and comfort, often causing irritation, abnormal discharge, and disruption of normal vaginal balance if left untreated. Common symptoms: Vaginal itching or burning Abnormal discharge Foul vaginal odor Common causes: Bacterial or fungal overgrowth Poor intimate hygiene Antibiotic use is disrupting vaginal flora 6. Menstrual Disorders Menstrual disorders include irregular, heavy, or painful periods and are common gynecological problems across age groups. Common symptoms: Missed or irregular cycles Excessive menstrual bleeding Severe menstrual cramps Common causes: Hormonal imbalance Thyroid disorders Stress or lifestyle factors 7. Ovarian Cysts Ovarian cysts are fluid-filled sacs on the ovaries and are often detected during routine gynecological evaluation. Common symptoms: Pelvic or lower abdominal pain Bloating or fullness Pain during menstrual cycles Common causes: Hormonal fluctuations Ovulation-related issues Underlying gynecological disorders 8. Cervical Dysplasia Cervical dysplasia involves abnormal changes in cervical cells and is considered a precancerous gynecological condition. Common symptoms: Often asymptomatic in early stages Abnormal vaginal bleeding Pain during intercourse Common causes: Human papillomavirus (HPV) infection Weak immune response Smoking 9. Infertility-Related Gynecological Disorders Several gynecological disorders directly affect fertility and reproductive function, making early diagnosis and proper gynecological treatment important for women planning pregnancy. Common symptoms: Difficulty conceiving Irregular ovulation Hormonal imbalance Common causes: PCOS Endometriosis Blocked fallopian tubes 10. Menopause-Related Gynecological Disorders Hormonal changes during menopause can lead to multiple gynecological problems affecting comfort and quality of life. Common symptoms: Hot flashes and night sweats Vaginal dryness Mood changes Common causes: Decline in estrogen levels Age-related hormonal changes Reduced ovarian function Treatment Options for Gynecological Disorders Treatment for gynecological disorders depends on the specific condition, symptom severity, age, and reproductive goals of the patient. Early and personalized gynecological treatment helps control symptoms and prevent complications. Common treatment options include: Medications and hormone therapy to regulate periods, control pain, and correct hormonal imbalances Lifestyle and dietary changes to manage conditions like PCOS and menstrual disorders Physiotherapy for pelvic floor strengthening and chronic pelvic pain relief Minimally invasive gynecological surgery for fibroids, endometriosis, or ovarian cysts Fertility treatments when gynecological disorders affect conception Timely treatment improves quality of life and long-term reproductive health. Who Is Affected by Gynecological Disorders? Gynecological disorders can affect women at different life stages due to
Non-Invasive Cardiology: Cost, Procedure, Benefits & When You Need It
Non-Invasive Cardiology: Cost, Procedure, Benefits & When You Need It Home / Heart-related problems often develop without clear symptoms, which makes early evaluation & treatment extremely important. Non-invasive cardiology focuses on diagnosing and monitoring heart conditions using safe cardiology tests that do not involve surgery or catheter-based procedures. Through techniques such as imaging and heart rhythm monitoring, non-invasive cardiology helps assess heart structure, blood flow, and cardiac function accurately. These methods allow cardiologists to detect heart disease early while minimizing risk and discomfort for patients. People searching for non-invasive cardiology often want clear knowledge about the procedure, the cardiology tests used, the benefits, the cost in India, and how it differs from invasive or interventional cardiology. This guide explains these aspects in a simple, patient-friendly way to support informed decisions. What Is Non-Invasive Cardiology? Non-invasive cardiology focuses on evaluating heart health using diagnostic tests that do not involve surgery, incisions, or instruments entering the blood vessels. These methods help cardiologists assess heart structure, function, and rhythm safely and painlessly. These tests help detect: Heart disease Heart valve abnormalities Rhythm disorders such as arrhythmias Reduced heart-pumping function Early signs of arterial blockage Because it carries minimal risk, non-invasive cardiology treatment is usually the first and most important step before considering invasive or interventional cardiology procedures. Common Cardiology Tests Used in Non-Invasive Cardiology Non-invasive cardiology relies on advanced yet safe cardiology tests to evaluate overall cardiac health, blood flow, and electrical activity of the heart. These tests help diagnose problems accurately without exposing patients to surgical stress. Key Non-Invasive Cardiology Tests Include: ECG (Electrocardiogram): Records the heart’s electrical signals to detect rhythm abnormalities Echocardiography (Echo Cardiology): Uses ultrasound to evaluate heart chambers, valves, and pumping strength Treadmill Test (TMT): Monitors heart performance during physical exertion Holter Monitoring: Continuously tracks heart rhythm over 24–48 hours Stress Echo: Identifies exercise-related heart problems not visible at rest These non-invasive cardiology tests help detect heart conditions early, guide treatment decisions, and reduce the need for invasive procedures. Tests Before Non-Invasive Cardiology Evaluation Before the beginning of non-invasive cardiology treatment, doctors conduct a detailed clinical review to choose the most appropriate cardiology tests. This step improves diagnostic accuracy and avoids unnecessary testing. Pre-evaluation usually includes: Review of medical history and current symptoms Blood pressure and cholesterol assessment Blood sugar level evaluation Family history of heart disease This structured evaluation ensures that non-invasive cardiology tests are correctly selected and interpreted, resulting in reliable diagnoses and effective heart care planning. Procedure of Non-Invasive Cardiology The procedure of non-invasive cardiology is designed to be simple, safe, and comfortable for patients. Most non-invasive cardiology evaluations are performed on an outpatient basis and do not require hospital admission. General steps include: Initial patient assessment, symptoms review, and vital sign checks Performing the recommended cardiology tests, such as ECG, echocardiography, or stress tests Recording heart images, rhythm, or exercise response Detailed clinical interpretation by an experienced cardiologist Guidance on non-invasive cardiology treatment, lifestyle changes, or further evaluation Most non-invasive cardiology procedures take 15 to 60 minutes, allowing patients to resume normal activities the same day. Benefits of Non-Invasive Cardiology Non-invasive cardiology offers significant advantages, particularly for patients who need early heart evaluation without surgical risk. It is often the first step in diagnosing and monitoring heart disease. Key benefits include: No surgery, injections, or hospital stay required Minimal discomfort with very low complication risk Early detection of heart disease and functional abnormalities Safe for elderly patients and those with existing medical conditions Helps avoid or delay unnecessary invasive cardiology procedures These advantages make non-invasive cardiology treatment a vital part of modern, patient-friendly heart care. Difference Between Invasive and Non-Invasive Cardiology The difference between invasive and non-invasive cardiology lies in the approach to heart evaluation. Non-invasive cardiology uses imaging and monitoring tests without surgery, while invasive cardiology involves catheter-based procedures for diagnosis or treatment. Aspect Non-Invasive Cardiology Invasive Cardiology Surgery Required No Yes Diagnostic Method Imaging & monitoring Catheter-based Risk Level Very low Moderate Recovery Time Same day Several days Usage Diagnosis & monitoring Treatment & intervention In most cases, non-invasive cardiology is used first, while invasive cardiology is recommended only when further intervention is necessary. Who Needs Non-Invasive Cardiology? Non-invasive cardiology is recommended for individuals who have symptoms or risk factors related to heart disease, even if the symptoms appear mild. You may need a non-invasive cardiology evaluation if you experience: Chest pain or shortness of breath – which may indicate reduced blood flow or early heart disease Palpitations or irregular heartbeat – often linked to rhythm disorders that require monitoring Fatigue during routine physical activity – a possible sign of reduced heart function High blood pressure or diabetes – conditions that significantly increase cardiac risk A family history of heart disease – genetic factors may raise the likelihood of heart problems Non-invasive cardiology tests are also widely used for routine heart screening, helping detect early cardiac abnormalities and guide timely treatment before serious complications develop. Non-Invasive Cardiology Treatment Approach The non-invasive cardiology treatment approach focuses on understanding heart function and managing risk without surgical intervention. It plays an important role in preventive and long-term heart care. Non-invasive cardiology treatment includes: Accurate diagnosis using cardiology tests Risk assessment for heart disease progression Ongoing monitoring of heart function Guiding medication, diet, and lifestyle changes Based on these findings, cardiologists can determine whether continued non-invasive care is sufficient or if invasive cardiology procedures are required. Non-Invasive Cardiology Cost in India The non-invasive cardiology cost in India is generally affordable and varies based on the type and number of diagnostic tests required. These tests help evaluate heart health without surgery, making them a cost-effective option for early diagnosis and routine screening. Approximate Cost Range: Individual tests: ₹1,500 – ₹15,000 per test Comprehensive non-invasive cardiology evaluation: ₹5,000 – ₹25,000 Cost Depends On: Type of cardiology test performed (ECG, echo cardiology, TMT, Holter, etc.) Technology and equipment used Number of tests required City location and healthcare facility standards Overall, non-invasive cardiology remains significantly more affordable than invasive
Difference Between Kidney Stone Pain and Appendix Pain
Difference Between Kidney Stone Pain and Appendix Pain Home / The difference between kidney stone pain and appendix pain is one of the most commonly searched health questions because both conditions cause sudden, severe abdominal pain that can confuse patients. People often panic when the pain starts, unsure whether they are experiencing kidney stone discomfort or an appendicitis emergency. Identifying the correct source of the pain is extremely important because the treatments for both conditions are completely different. While kidney stones usually cause radiating back pain and difficulty in passing urine, appendix pain often begins near the navel and gradually shifts to the lower right side of the abdomen. In this blog, we will explain the key differences between kidney stone pain and appendix pain in a simple, clear manner. We will also cover symptoms, causes, diagnosis, risks, and treatment options for both conditions. If you are experiencing severe abdominal pain, Numed Hospital, Greater Noida West, provides expert emergency care and advanced diagnostics to ensure quick and accurate treatment. Understanding Appendix Pain Appendix pain occurs when the appendix — a small, finger-shaped pouch attached to the large intestine — becomes swollen and infected. This condition is called appendicitis and is a medical emergency that requires immediate treatment. Appendix pain usually starts near the belly button and then moves to the lower right side of the abdomen. The pain becomes sharper and worse over time. Unlike kidney stone pain, appendix pain does not move around the body. It continuously worsens, especially during coughing, walking, or pressing the abdomen. Fever, vomiting, loss of appetite, constipation, or diarrhea are common symptoms. If untreated, the appendix may burst, leading to a life-threatening condition called peritonitis. That is why recognizing appendix pain early is extremely important. Difference between appendicitis and kidney stones Appendicitis and Kidney Stones are different conditions mainly in how their pain and symptoms appear. Appendicitis usually starts with pain near the navel that shifts to the lower right abdomen and becomes steady and more severe over time, often with fever, nausea, and loss of appetite; movement typically makes the pain worse, so the person prefers to stay still. In contrast, kidney stones cause sharp, intense pain that begins in the side or back and may move toward the groin, coming in waves, and patients often feel restless due to the pain; it is commonly associated with urinary symptoms like burning or blood in urine. Pain Location: The Key Distinguishing Factor Pain location is one of the clearest indicators: Kidney Stone Pain:Starts in the back or side (flank region). Moves towards the lower abdomen or groin as the stone travels through the urinary tract. The pain radiates and changes position. Appendix Pain:Starts near the belly button and then shifts to the lower right side. It does not radiate and stays in one specific area. This shift from central to right lower abdomen is a classic sign of appendicitis. Patients often describe kidney stone pain as unbearable, stabbing pain, while appendix pain is more constant, sharp, and progressively worsening. Nature of the Pain Kidney stone pain comes in intervals. It intensifies when the stone moves and decreases when it stops. This wave-like pattern is called “colicky pain.” Appendix pain, on the other hand, is steady. There are no waves or relief moments. Once it begins, it continuously worsens, especially when you move, walk, cough, or touch the abdomen. Kidney Stones vs Appendicitis Feature Kidney Stones Appendicitis Pain Location Side/back → may move to lower abdomen or groin Starts near navel → shifts to lower right abdomen Pain Type Sharp, severe, comes in waves Steady, worsening pain Movement Effect Patient keeps moving due to pain Movement makes pain worse (patient stays still) Urine Symptoms Burning, blood in urine Usually no urinary issues Digestive Symptoms Nausea possible Nausea, vomiting, loss of appetite common Fever Rare (unless infection) Common (mild fever) Associated Symptoms: Comparing Both Conditions Kidney stones come with symptoms like burning urination, blood in urine, nausea, and frequent urge to pass urine. Appendix pain is linked to digestive symptoms like loss of appetite, vomiting, mild fever, constipation, or diarrhea. The abdomen becomes tender, and even slight pressure causes intense pain. A major difference is that kidney stones affect the urinary system while appendicitis affects the digestive system. How Doctors Diagnose Kidney Stone Pain and Appendix Pain Accurate diagnosis is crucial because both conditions require different treatments. At Numed Hospital, doctors perform a combination of physical examinations and advanced imaging tests to identify the exact cause of abdominal pain. For suspected kidney stones, ultrasound, urine tests, and CT scans help locate the stone and determine its size and position. For appendicitis, doctors check abdominal tenderness and perform ultrasound or CT abdomen scans to confirm appendix inflammation. Early diagnosis prevents complications and ensures faster recovery. Risks and Complications Kidney stones can lead to urinary tract infections, kidney blockage, severe infections, and long-term kidney damage if untreated. Stones may grow larger and become impossible to pass without medical support. Appendicitis is more dangerous because a ruptured appendix can spread infection throughout the abdomen, leading to peritonitis and sepsis. This is a life-threatening condition that requires emergency surgery. Understanding the seriousness of these complications shows why abdominal pain should never be ignored. what can be mistaken for kidney stones? explain appendicitis symptoms Several conditions feel similar to kidney stone pain, such as: Urinary Tract Infection (UTI) – burning urination, frequent urge Appendicitis – pain starting near navel, moving to lower right side Gallstones – pain in upper right abdomen Muscle strain – back pain after movement or lifting Irritable Bowel Syndrome – cramping with bowel changes Kidney infection – fever + back pain (more severe than stones) Treatment Options for Kidney Stone Pain Treatment depends on the stone’s size and location. Small stones may pass naturally with increased water intake and pain medication. Doctors may also prescribe medicines that relax the ureter muscles to help stones move. Larger stones may require shockwave therapy, laser treatment, or surgical procedures.
Irregular Periods After 30 – Causes Most Women Ignore

Irregular Periods After 30 – Causes Most Women Ignore Home / Irregular periods after the age of 30 are far more common than most women realize. While an occasional delay or early cycle may not seem serious, frequent irregularity can indicate underlying health conditions that often go unnoticed. Women in their 30s juggle career, family, stress, lifestyle changes, and hormonal shifts — all of which influence the menstrual cycle. But ignoring irregular periods can delay the diagnosis of important health issues like hormonal imbalance, thyroid disorders, PCOS, stress-related problems, or nutritional deficiencies. In this blog, we will explore why irregular periods become more common after 30, the hidden causes women often ignore, when to seek medical help, and how Numed Super Speciality Hospital, the best multispeciality hospital in Noida Extension, supports women with advanced gynaecology care. Understanding What “Irregular Periods” Really Mean A normal menstrual cycle typically ranges between 24 to 35 days. Periods are considered irregular when: Your cycle length varies every month You miss periods frequently Your periods come earlier or later than expected Bleeding is unusually heavy or too light Your cycle suddenly becomes erratic after being regular for years For women above 30, these irregularities often signal hormonal or lifestyle-related disruptions. Why Irregular Periods Increase After Age 30 Your 30s are a transformative decade for your body. Hormones fluctuate due to stress, lifestyle changes, reproductive planning, metabolism shifts, and age-related hormonal transitions. Even slight hormonal imbalance can disturb the menstrual cycle. Below are the most common and often ignored causes of irregular periods after 30, explained cleanly and clearly. 1. Hormonal Imbalance — The Most Overlooked Cause Hormones like estrogen, progesterone, and LH (luteinizing hormone) play the biggest role in regulating your cycle. Any imbalance can disrupt ovulation and change your period schedule. Common hormonal triggers include: Stress Poor sleep Excessive travel Sudden lifestyle changes Weight fluctuations Using emergency contraceptives This is one of the top reasons for irregular menstrual cycle in your 30s. 2. Polycystic Ovary Syndrome (PCOS) PCOS is extremely common among young women today, especially after 30.Symptoms include: Irregular or missed periods Excess facial/body hair Acne or oily skin Weight gain Difficulty conceiving PCOS disrupts ovulation, making cycles unpredictable. It is one of the most searched health concerns among women and a leading cause of irregular periods. 3. Thyroid Imbalance (Hypothyroidism or Hyperthyroidism) Your thyroid gland controls metabolism and reproductive hormones. Even mild thyroid imbalance can cause: Irregular cycles Heavy or very light bleeding Mood changes Weight problems Fatigue Women in their 30s are at higher risk for thyroid disorders due to hormonal transitions, stress, and nutritional issues. 4. High Stress Levels Stress releases cortisol — a hormone that directly interferes with the reproductive system.Common stress triggers: Work pressure Relationship stress Parenting responsibilities Financial worries Lack of rest 5. Rapid Weight Gain or Weight Loss Sudden changes in body fat percentage affect estrogen production. Being underweight can stop periods completely. Being overweight can cause heavy, painful, or irregular cycles. Maintaining a healthy weight is essential to regulate hormones naturally. 6. Excessive Exercise Many women after 30 start intense fitness routines for weight management. But excessive workouts, low-calorie diets, or overtraining can lead to exercise-induced amenorrhea — missing periods due to stress on the body. 7. Perimenopause (Early Hormonal Changes) Perimenopause can begin in the early 30s for some women, especially due to genetics, stress, or medical conditions.Symptoms include: Irregular periods Hot flashes Mood swings Sleep problems This transitional phase causes fluctuations in estrogen and progesterone. 8. Birth Control Pills or Hormonal Devices Stopping or starting birth control pills, hormonal IUDs, or emergency contraceptives can cause temporary irregular cycles. This is normal but should be monitored. 9. Underlying Medical Conditions Certain conditions can also contribute: Fibroids Endometriosis Pelvic infections Chronic illnesses Diabetes or insulin resistance Ignoring repeated irregular cycles may delay important diagnosis. 10. Nutritional Deficiencies Deficiency of iron, vitamin D, vitamin B12, and omega-3 can impact hormone production, leading to irregular cycles.Women in their 30s often experience deficiencies due to busy lifestyles. When Should You See a Doctor? Seek medical help if: You miss periods for 2–3 months Bleeding becomes unusually heavy Your cycle remains unpredictable for over six months You experience severe pain, fatigue, or mood changes You’re trying to conceive but cycles are irregular Your periods suddenly change after years of regular cycles These symptoms indicate that your hormones or reproductive system need attention. How Irregular Periods Affect Long-Term Health Ignoring irregular periods can lead to: Fertility issues Hormonal imbalance Difficulty conceiving Weight problems Insulin resistance PCOS progression Thyroid complications Endometrial problems Timely diagnosis helps avoid long-term complications and supports reproductive health. How to Regulate Your Periods Naturally (Clean & Simple Tips) Maintain a consistent sleep schedule Reduce caffeine and sugar intake Manage stress through breathing or meditation Eat a balanced diet rich in protein, iron & healthy fats Exercise moderately Stay hydrated Avoid smoking & limit alcohol Maintain a healthy weight These simple habits support natural hormonal balance. Why Choose Numed Hospital for Irregular Period Concerns? Numed Super Speciality Hospital, Noida Extension, provides expert and compassionate care for all women’s health issues.As the best multispeciality hospital in Noida Extension, Numed offers: Experienced gynaecologists Advanced diagnostic facilities Hormonal evaluation Ultrasound & fertility assessments PCOS and thyroid management Personalized treatment plans 24×7 emergency support Whether your irregular periods are due to hormonal imbalance, thyroid issues, PCOS, stress, or lifestyle factors, Numed Hospital provides complete care under one roof. Your health deserves timely attention — and Numed ensures safe, accurate, and advanced women’s healthcare. Final Thoughts Irregular periods after 30 are common but not “normal.” They are your body’s way of signaling hormonal imbalance or lifestyle stress. The key is not to ignore them. Understanding your cycle, seeking timely care, and maintaining healthy habits can prevent long-term complications and protect your reproductive health. If you’re experiencing irregular periods, heavy bleeding, missed cycles, or fertility concerns, don’t delay professional care.Visit Numed Super Speciality Hospital, Noida Extension, for expert diagnosis and complete gynaecology support.
Why Low Water Intake Harms Your Health

Why Low Water Intake Harms Your Health Home / Why Low Water Intake Harms Your Health is a question that deserves far more attention than it usually gets. Water is not just a drink — it’s the most essential element that keeps your body functioning smoothly every single day. Still, a large portion of people unknowingly drink far less water than their body actually needs. Dehydration rarely shows dramatic symptoms in the beginning, which is why it goes unnoticed. But with time, this habit silently affects your kidneys, brain, skin, energy levels, heart, digestion, and overall long-term health. Most people believe dehydration only happens when you are in the sun or sweating excessively. But in reality, chronic dehydration happens indoors, in air-conditioned offices, during long working hours, while skipping meals, or simply because you don’t feel thirsty. Your body needs water even when you’re sitting still, sleeping, or resting. When that daily requirement is ignored, internal systems start compensating — and that’s where problems begin. In this extended guide, you’ll understand how dehydration affects your body, why even “mild dehydration” can disrupt major functions, what long-term risks you should be aware of, and how to restore hydration health in simple, effective ways. You’ll also know when dehydration becomes a medical concern and why Numed Hospital, Noida Extension, is trusted for hydration-related health issues. How Low Water Intake Affects Your Body from Within The human body is made of nearly 60% water. Your blood, organs, and tissues all depend on water to maintain balance. When your water intake drops, the body immediately tries to survive with whatever limited fluid is available. This is called compensatory dehydration, and it silently stresses your internal organs. Your kidneys begin concentrating urine because they’re trying to save water. This makes your urine darker and more acidic. Your brain receives less oxygen-rich blood, which is why you feel tired, slow, or unfocused. Your digestion slows down because water is needed to break down food, move waste, and maintain healthy bowel movements. Even your joints begin losing lubrication — which many people mistakenly label as “age-related pain.” Skin is another area affected early. Many people spend money on creams and treatments, but the most important moisturizer is water. Without proper hydration, your skin loses elasticity, making it look dull, rough, and more prone to wrinkles. In simple terms:Low hydration forces your body to work harder, but perform worse. And unlike sudden dehydration, this type of chronic dehydration builds over weeks, months, and eventually years. Why Low Water Intake Leads to Fatigue & Low Energy One of the earliest signs of dehydration is a sudden drop in daily energy. Many people assume their tiredness is due to low sleep, workload, or stress — but dehydration is often the hidden reason. When your water intake is low, your blood becomes slightly thicker. This slows circulation, meaning your cells receive less oxygen and nutrients. As a result, even normal activities feel tiring. You may feel mentally dull, sleepy, or unable to focus. Your brain needs proper hydration for electrical signals to function smoothly. Even a 1–2% drop in hydration levels can reduce cognitive performance — something research strongly supports. In short:If you feel tired even after resting, dehydration might be the culprit. Impact on Digestion & Gut Health Digestion heavily depends on water. Without enough hydration: Stomach acid becomes stronger → causing acidity and heartburn Intestinal movement slows → causing constipation and bloating Nutrient absorption reduces → making you feel weak despite eating well People often assume they need medicine for constipation, acidity, or sluggish digestion, but increasing water intake is one of the simplest and most natural solutions. Effect on Kidneys, Urinary System & Toxins At Numed Hospital, obesity diagnosis is done through a detailed medical evaluation instead of just checking BMI. Doctors assess body fat percentage, waist-to-hip ratio, metabolic rate, thyroid levels, insulin resistance, lipid profile, liver status, and hormonal health. These tests help identify the exact cause of weight gain and allow experts to create a personalized treatment plan. Understanding whether obesity is lifestyle-related, hormone-related, or stress-related is the key to successful treatment. Long-Term Health Risks You Should Not Ignore If dehydration becomes your daily habit, several long-term problems can develop gradually: 1. Kidney Stones Without enough water, minerals like calcium and uric acid crystallize and form stones. They can become extremely painful and require medical treatment. 2. Frequent UTIs Insufficient water does not flush bacteria from the urinary tract. This allows infections to develop, especially in women. 3. Chronic Constipation Dehydration makes stools hard and painful to pass, leading to piles or fissures. 4. Early Skin Ageing Without hydration, the skin loses elasticity, causing wrinkles, pigmentation, and dryness. 5. Joint Pain & Stiffness Your joints contain synovial fluid — mostly water. Low hydration reduces lubrication. 6. Heart Stress Thicker blood makes your heart pump harder, increasing long-term cardiac strain. 7. Poor Focus & Mood Issues Dehydration affects neurotransmitters, leading to irritability, mood swings, and anxiety. With time, these issues may require medical attention — which is why hydration should never be ignored. How Much Water Do You Actually Need? General hydration needs depend on weather, activity level, and body composition, but an average adult requires: 2.5 to 3.5 liters per day You may need more if you: Exercise regularly Drink a lot of tea, coffee, or soda Live in hot weather Eat high-sodium foods Are pregnant or breastfeeding The simplest way to check hydration is through urine color: Light/clear = properly hydrated Dark yellow = dehydrated Listening to your body is important, but relying only on “thirst” is not enough — by the time you feel thirsty, your body is already dehydrated. Simple Daily Habits to Improve Hydration Hydration is easy to fix with small, consistent steps. Start your morning with a glass of water. Carry a bottle during work hours. Sip water at regular intervals. Eat fruits, salads, soups, coconut water, and herbal drinks that naturally hydrate the body. Reduce excess caffeine and
Obesity – Causes, Symptoms & Treatment Options

Obesity – Causes, Symptoms & Treatment Options Home / Obesity is one of the most rapidly increasing health concerns in today’s world. It is often misunderstood as just “weight gain,” but medically, obesity is a chronic metabolic condition that affects almost every system of the body. When excess fat accumulates beyond healthy levels, it starts interfering with hormones, digestion, heart function, liver health, joint mobility, and even mental well-being. In India, the combination of fast food culture, long sitting hours, stress, and hormonal imbalance has made obesity extremely common. This blog explains obesity in a simple, easy-to-understand way while covering its causes, symptoms, complications, and treatment options. If you or someone you know is struggling with weight issues, Numed Hospital, Greater Noida West provides comprehensive and personalized obesity care. What Is Obesity? Obesity is defined as an excessive accumulation of body fat that negatively impacts health. Doctors primarily use the Body Mass Index (BMI) to categorize weight levels, but BMI alone does not give the complete picture. Other factors such as waist circumference, body fat percentage, hormonal activity, and metabolism also play a major role. People with high belly fat (visceral fat) are at a greater risk of lifestyle diseases like diabetes, high blood pressure, fatty liver, heart attack, and infertility. That is why obesity is not a cosmetic issue; it is a medical condition that requires early management. Causes of Obesity Obesity does not happen overnight. It develops gradually due to a mix of lifestyle habits, biological factors, hormones, and mental health patterns. The most common cause is an unhealthy diet—foods high in sugar, unhealthy fats, fried snacks, fast food, and sugary beverages lead to rapid fat storage and higher insulin levels. Portion sizes have also increased dramatically in modern diets, causing more calorie intake than the body can burn. Another major reason is a sedentary lifestyle. Many people spend long hours sitting at work, on screens, or while commuting. Minimal physical activity slows down the metabolism, reduces muscle mass, and increases fat accumulation. In addition to lifestyle, hormonal imbalances significantly contribute to weight gain. Conditions such as hypothyroidism, PCOS, insulin resistance, and increased cortisol due to stress make the body hold on to fat even when a person is trying to eat less. Genetics also play a role. If obesity runs in your family, you may naturally have a slower metabolism or higher appetite levels. Stress eating is another reason many people gain weight. Emotional hunger often leads to cravings for high-calorie comfort foods, especially at night. Certain medicines—like steroids, antidepressants, and some diabetes medications—can also lead to weight gain. Together, these factors create the perfect environment for obesity to develop and worsen. Symptoms of Obesity If obesity is not treated early, it can lead to several long-term health problems. Excess fat around the organs increases the risk of Type 2 diabetes, high blood pressure, high cholesterol, heart attack, and stroke. Fatty liver disease is extremely common in obese individuals because the liver starts storing fat and becomes inflamed. Fertility issues are also linked to obesity, affecting both men and women. Joint issues such as osteoarthritis become more severe due to excess weight. Many people also develop sleep apnea, depression, low immunity, and even kidney-related problems. Treating obesity early can prevent these complications and drastically improve quality of life. Diagnosis of Obesity At Numed Hospital, obesity diagnosis is done through a detailed medical evaluation instead of just checking BMI. Doctors assess body fat percentage, waist-to-hip ratio, metabolic rate, thyroid levels, insulin resistance, lipid profile, liver status, and hormonal health. These tests help identify the exact cause of weight gain and allow experts to create a personalized treatment plan. Understanding whether obesity is lifestyle-related, hormone-related, or stress-related is the key to successful treatment. Health Complications Linked to Obesity Obesity shows many early signs, but people often ignore them. One of the most noticeable symptoms is steady or rapid weight gain without any clear reason. An increasing waistline is also a strong indicator, especially when the waist measurement crosses medically safe limits. People with obesity often feel breathless during small activities because excess fat puts pressure on the lungs and heart. Constant fatigue, low energy, and a feeling of heaviness during the day are also common. Obesity affects the joints too. Extra weight increases the load on the knees, lower back, and spine, causing chronic pain and limited movement. Many people experience disturbed sleep or loud snoring due to fat around the neck area, which blocks the airway—a condition known as sleep apnea. Women with obesity often face irregular periods, hormonal imbalance, and PCOS-related symptoms. Along with physical issues, obesity also impacts emotional health, reducing self-confidence and increasing stress or anxiety. Treatment Options for Obesity Obesity treatment is not about crash diets or extreme workouts. It requires a scientific and step-by-step approach that targets the root cause. The first line of treatment is lifestyle modification. This includes a balanced, calorie-controlled diet that is rich in protein, fiber, and essential nutrients while reducing sugar, fried foods, and processed carbs. Regular physical activity—whether walking, yoga, gym, or home exercises—helps improve metabolism and gradually burns fat. Proper sleep and stress management are equally important because hormonal balance plays a vital role in weight control. At Numed Hospital, Medical Nutrition Therapy (MNT) is offered by expert dieticians who design personalized diet plans based on your body’s requirements. These diets are safe, sustainable, and designed to support long-term weight management. In some cases, doctors may prescribe weight-loss medications to control appetite, improve insulin sensitivity, and support fat burning. These medicines are only given after proper evaluation. For people with hormonal disorders like hypothyroidism or PCOS, treating the underlying hormonal imbalance becomes the priority. Once hormones are stabilized, weight loss becomes more natural and effective. Physiotherapy is also helpful for individuals with knee pain or mobility issues, as it strengthens joints and makes movement easier. In severe obesity cases where BMI is above 35 or 40 and lifestyle changes are not enough, bariatric surgery may
How to Stop OCD Thoughts Naturally: A Complete, Simple & Supportive Guide

How to Stop OCD Thoughts Naturally: Simple & Effective Methods Home / How to stop OCD thoughts naturally becomes an important question when intrusive, repetitive thoughts start affecting your peace of mind. Living with obsessive thoughts can feel overwhelming, exhausting, and even isolating. Many people silently struggle with intrusive ideas that repeat again and again, causing stress and interfering with daily life. If you are someone searching for how to stop OCD thoughts naturally, it means you’re looking for safe, gentle, and realistic ways to regain control without depending solely on medication. This guide explains practical strategies, lifestyle changes, and mindset shifts that can genuinely help you manage obsessive thoughts in a healthy, natural, and sustainable way. How to stop OCD thoughts naturally becomes an important question when intrusive, repetitive thoughts start affecting your peace of mind. Living with obsessive thoughts can feel overwhelming, exhausting, and even isolating. Many people silently struggle with intrusive ideas that repeat again and again, causing stress and interfering with daily life. If you are someone searching for how to stop OCD thoughts naturally, it means you’re looking for safe, gentle, and realistic ways to regain control without depending solely on medication. This guide explains practical strategies, lifestyle changes, and mindset shifts that can genuinely help you manage obsessive thoughts in a healthy, natural, and sustainable way. Understanding OCD Thoughts in Simple Words Before learning how to stop OCD thoughts naturally, it’s important to understand what these thoughts really are.OCD thoughts are unwanted, intrusive ideas, images, or doubts that keep repeating in your mind. These thoughts feel disturbing and trigger anxiety, fear, or discomfort. Common examples include: Feeling worried all the time about dirt or cleanliness Constantly checking things like locks, gas knobs, or switches Fear of harming yourself or others Needing things to be “perfect” or in the “right order” Repetitive unwanted images Uncomfortable thoughts that go against your true nature These thoughts are not your fault and don’t mean anything about you as a person. They are simply mental noise created by anxiety and habit loops in the brain. Ways to Stop OCD Thoughts Naturally Below are the most effective, research-backed natural methods to manage intrusive thoughts. Each of these can work differently for different people, so the best approach is to try them consistently and patiently. 1. Label the Thought Instead of Fighting It One of the most powerful ways to learn how to stop OCD thoughts naturally is to reduce resistance. Instead of reacting with fear, try saying to yourself: “This is just an OCD thought.” “This is a mental habit, not reality.” When you label it instead of fighting it, the thought starts losing its power. The most common type, occurring when intestine pushes into the groin area. More common in men. 2. Practice Deep Breathing to Calm Your Brain OCD thoughts get stronger when your mind is stressed.Deep breathing helps your brain shift from panic mode to relaxation mode. Try this simple method: Inhale for 4 seconds Hold for 2 seconds Exhale for 6 seconds Doing this 8–10 times reduces anxiety and weakens intrusive thoughts. Occurs near the belly button and is common in infants, pregnant women, and overweight individuals. 3. Use the “Delayed Response” Technique When an intrusive thought appears, instead of reacting immediately, say: “I will think about this later.” This breaks the automatic cycle of reacting to every OCD trigger and helps you understand how to stop OCD thoughts naturally by creating mental distance. 4. Try Mindfulness to Stay in the Present Moment Mindfulness means observing your thoughts without judging them. A simple daily practice: Sit quietly Focus on your breathing Notice any thoughts that appear Let them pass like clouds Over time, the brain becomes less reactive, and OCD thoughts lose their intensity. 5. Ground Yourself with the 5-4-3-2-1 Method OCD thoughts can make you feel trapped in your mind.Grounding techniques help you come back into the present. Look around and identify: 5 things you can see 4 things you can touch 3 things you can hear 2 things you can smell 1 thing you can taste This method is simple but extremely effective for calming the mind naturally. 6. Engage in Physical Activity Exercise releases natural chemicals in your brain that reduce anxiety and obsessive thoughts. Ideal activities include: Walking Yoga Cycling Stretching Dancing Just 20–30 minutes a day can significantly improve your mental balance. 7. Reduce Caffeine and Sugar Symptoms vary depending on the part of the brain involved. Common signs include: Sudden jerking movements Loss of awareness Staring spells Confusion after an episode Uncontrolled shaking Temporary loss of memory If someone experiences repeated seizures, they should immediately consult a neurologist for epilepsy treatment in Delhi. 8. Create a “Thought Record” Journal Writing down intrusive thoughts helps you organize your mind and separate fear from facts. You can write: What the thought was What triggered it How you reacted A more balanced reply This technique turns overwhelming thoughts into manageable information. 9. Spend Time in Nature Nature has a calming effect on the brain.Even 10 minutes of: Parks Gardens Sunlight Fresh air can reduce mental stress and interrupt obsessive thought patterns. 10. Practice Self-Compassion Nature has a calming effect on the brain.Even 10 minutes of: Parks Gardens Sunlight Fresh air can reduce mental stress and interrupt obsessive thought patterns. 11. Improve Sleep Quality Poor sleep increases anxiety and makes intrusive thoughts stronger. Follow these tips: Maintain a sleep schedule Avoid screens 30 minutes before bed Keep your room cool and dark Don’t consume caffeine after evening Good sleep naturally improves emotional strength. 12. Use the “Acceptance” Approach The more you fight an OCD thought, the stronger it becomes. Try accepting it like this: “I am noticing this thought. It’s uncomfortable, but it’s okay.” Acceptance teaches your brain not to panic, and that is one of the best natural ways to break the OCD cycle. When to Seek Professional Help Natural methods are powerful, but if intrusive thoughts are: Affecting your daily routine
Hernia – Types, Symptoms, Causes & Laparoscopic Treatment
Hernia – Types, Symptoms, Causes & Laparoscopic Treatment Home / A hernia is a common medical condition in which an internal organ pushes through a weak spot in the muscles or abdominal wall. Hernias can appear as a bulge in the abdomen, groin, or upper thigh and often become more noticeable while coughing, bending, standing, or lifting heavy objects. Early diagnosis and proper treatment are essential to avoid complications like strangulation or obstruction. If you’re searching for what a hernia is, types of hernia, hernia symptoms, causes, high-risk factors, or advanced laparoscopic hernia treatment, this detailed guide covers everything in simple, easy-to-understand language. Numed Hospital — a leading hospital in Noida Extension — offers advanced laparoscopic hernia repair performed by expert surgeons using minimally invasive techniques. What Is a Hernia? A hernia develops when a portion of tissue or intestine pushes through a weakened area of the surrounding muscle. The bulge may be soft or firm and can increase in size over time. Hernias do not heal on their own and usually require medical attention to avoid complications. The most commonly affected areas are: Abdomen Groin (inguinal region) Upper thigh Belly button Diaphragm Hernias can cause discomfort, pain, and digestive issues depending on the severity. In some cases, a hernia may be painless initially but become painful as it enlarges or gets trapped. Causes of Hernia Hernias can occur due to multiple factors. Understanding the root causes helps in prevention and early detection. Major Causes of Hernia: Heavy lifting: Repeated lifting of heavy weights puts pressure on the abdominal wall. Chronic coughing: Persistent cough from smoking, asthma, or lung issues can weaken muscles. Straining during bowel movements: Severe constipation increases abdominal pressure. Pregnancy: Increased abdominal pressure causes muscle stretching. Obesity: Excess body weight weakens muscles over time. Previous surgeries: Incision sites may become weak and result in incisional hernia. Aging: Natural weakening of abdominal muscles. Genetic muscle weakness: Some people are born with weaker abdominal walls. Anyone can develop a hernia, but people who smoke, lift heavy weights, or have chronic coughs are at higher risk. Symptoms of a Hernia Recognizing hernia symptoms early helps prevent complications such as obstruction or strangulation. Common Symptoms of Hernia: A visible bulge in the abdomen, groin, or navel Pain or discomfort while lifting, bending, or coughing Heaviness or pressure in the abdominal area Burning or aching sensation at the bulge Difficulty standing for long periods Swelling or pain that worsens during physical activity In severe cases: nausea, vomiting, or inability to pass gas (emergency signs) If any of these hernia symptoms appear, it is important to seek medical attention immediately. Types of Hernia Hernias are classified based on their location. Understanding types helps determine the correct treatment plan. 1. Inguinal Hernia (Groin Hernia) The most common type, occurring when intestine pushes into the groin area. More common in men. 2. Umbilical Hernia Occurs near the belly button and is common in infants, pregnant women, and overweight individuals. 3. Incisional Hernia Happens at the site of previous surgical cuts where the muscle wall is weak. 4. Hiatal Hernia The upper part of the stomach pushes through the diaphragm into the chest. Causes heartburn and acidity. 5. Femoral Hernia Appears in the upper thigh, more common in women, and may lead to serious complications if untreated.The upper part of the stomach pushes through the diaphragm into the chest. Causes heartburn and acidity. 6. Epigastric Hernia Occurs between the rib cage and belly button, formed due to weakness in the upper abdominal muscles. How Hernias Are Diagnosed Symptoms vary depending on the part of the brain involved. Common signs include: Sudden jerking movements Loss of awareness Staring spells Confusion after an episode Uncontrolled shaking Temporary loss of memory If someone experiences repeated seizures, they should immediately consult a neurologist for epilepsy treatment in Delhi. Hernia Treatment Options Hernias do not go away on their own. Treatment depends on the type, severity, and progression. Non-Surgical Treatment (Limited Cases) Non-surgical methods may help temporarily but do not cure hernias. Common approaches: Lifestyle modifications Avoiding heavy lifting Weight management Hernia belts (temporary relief, NOT a cure) These are not permanent solutions. Surgical Treatment for Hernia Surgical repair is the only complete and permanent treatment for hernia. Surgical Options: Open Hernia Repair: Traditional surgery with a larger incision. Laparoscopic Hernia Repair: Minimally invasive, faster recovery, less pain. Laparoscopic repair is now the gold standard for most hernia types. Laparoscopic Hernia Treatment (Minimally Invasive Surgery) Laparoscopic surgery uses small incisions and a camera-guided technique to repair the hernia. It is considered the safest and most advanced treatment for hernia. Benefits of Laparoscopic Hernia Surgery: Minimal pain Faster recovery Small or no visible scars Reduced hospital stay Minimal blood loss Lower risk of recurrence Quick return to normal activities At Numed Hospital — a trusted hospital in Noida Extension, advanced laparoscopic hernia repair is performed by experienced surgeons using modern, high-precision equipment. Hernia Recovery Time Recovery time depends on the type of surgery and the patient’s overall health. Typical Hernia Recovery Timeline: 1–3 Days: Pain and swelling reduce 1 Week: Walking comfortably, minimal discomfort 2 Weeks: Can return to light work and activities 4–6 Weeks: Normal routine, exercise gradually resumes 6–12 Weeks: Complete internal healing Laparoscopic surgery speeds up recovery compared to open surgery. Preventing Hernia Although some hernias cannot be prevented, lifestyle changes can significantly reduce the risk. Prevention Tips: Maintain a healthy weight Avoid heavy lifting or use proper lifting techniques Treat chronic coughs early Include core strengthening exercises Eat fiber-rich foods to avoid constipation Quit smoking Manage diabetes and obesity Stay active to maintain muscle strength Strong abdominal muscles can help prevent hernias from developing or worsening. When to See a Doctor Immediately? Some hernias can become life-threatening if they become “strangulated” or “obstructed.” Seek immediate medical help if you notice: Severe abdominal pain Bulge that becomes hard or cannot be pushed back Nausea or vomiting Fever with swelling Inability to pass stool or gas Sudden increase in

